We work in some of the most climate-vulnerable settings in the world, responding to many of the world’s most urgent crises – conflict, extreme weather events, disease outbreaks, and displacement. These are settings where people already lack access to, or are excluded from, basic healthcare. These people are also the least responsible for the emissions that drive climate change. But the climate emergency aggravates some humanitarian crises and their subsequent healthcare consequences, which impact on people in these vulnerable settings the most.
As a medical organisation, it is beyond our field of expertise to define what causes many of the events that we then respond to. And while our teams in some places have noticed changes over the years, existing scientific evidence clearly points out that we will be seeing further rising temperatures and sea levels, and more frequent and intense extreme weather events.
Learn how we are mitigating our own contribution to the climate emergency and reducing our carbon footprint.
What are we seeing and doing?


When the climate warms and rainfall patterns change, mosquitoes – which transmit diseases such as malaria and dengue fever – breed more quickly and survive in places where they were not previously found, exposing more people to these deadly diseases. In Democratic Republic of Congo, malaria causes four times more deaths per year than conflict, meningitis, cholera, measles and respiratory diseases combined.

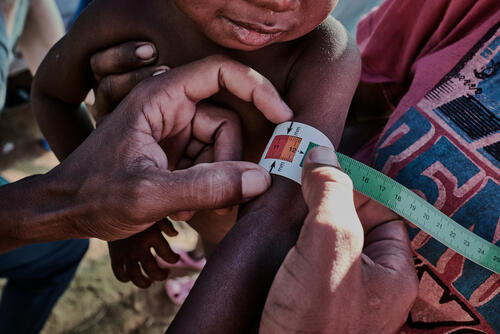
Increases in temperature, heat waves, droughts, and floods impact malnutrition in many places we work. In Niamey, Niger, where rains have brought floods and wiped-out crops, our teams have observed and responded, over the past two years, to increases in malnutrition cases. In southern Madagascar, consecutive years of drought have severely affected harvests and access to food, causing an acute food and nutrition crisis, leaving thousands of children severely ill and pushing entire families into extreme poverty.


Across the Sahel, in sub-Saharan Africa, climate change has contributed to an imbalance of land available to livestock herders and farmers. The competition over resources and the authorities’ inability to negotiate access to land have resulted in conflict between the two groups, adding to the violence and insecurity across the region, to which we respond to the consequences of by providing medical care. Conflict, in turn, often causes people to become displaced.


More frequent and serious extreme weather events increase the risk of injury, infectious disease, and malnutrition. A severe consequence of weather events like flooding, hurricanes, and cyclones is displacement. As people lose or leave their homes because of extreme weather, they are forced on the move. Millions of people are already displaced because of conditions that have been exacerbated by climate change. Throughout 2024, our teams responded to consistent flooding in areas around Old Fangak, South Sudan, which has inundated surrounding villages and displacing thousands of people.

Climate change affects all of us
Climate change affects all of us
Climate change - or the climate emergency - affects all of us, in direct and indirect ways. It impacts diseases such as malaria and malnutrition, and can contribute to conflict and displacement. The climate crisis is also a health and humanitarian crisis.




