While over 4.8 million people have managed to return home, around 1.1 million people remain displaced across 18 governorates*. Both returnees and those still displaced struggle to access basic services and job opportunities.
The healthcare system is unable to fulfil the needs of people, which is exacerbated by the shortages of specialist healthcare workers and drugs.
Our teams in Iraq continue to bridge the most pressing gaps in access to healthcare in four governorates. We provide general, maternal, neonatal, and mental healthcare, in addition to surgical procedures, post-operative care and rehabilitation, treatment for non-communicable diseases and emergency medical care.
*http://iraqdtm.iom.int/ - IOM
Why are we here?


MSF provides antenatal and postnatal care, neonatal and paediatric care, as well as family planning services. We assist births, including those with complications; our teams in Mosul and Sinjar assisted a total of 14,442 births in 2020. We also support the maternity department, at the Hawija General Hospital in Kirkuk, with emergency obstetric and neonatal care.

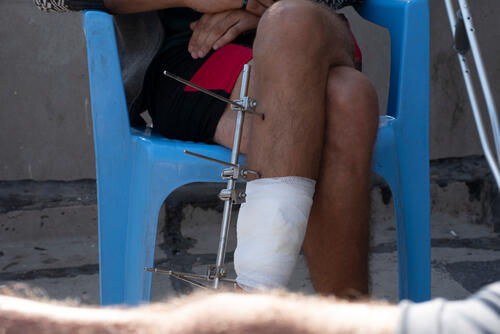
Many patients with physical injuries need specialised care. MSF provides surgical and rehabilitative care at Al-Wahda hospital in Mosul. We also run a medical rehabilitation centre in Baghdad, aiming to reduce long-term physical and psychological impairment of trauma patients through early physiotherapy, nursing care, pain management and mental health services care. Even after surgery, we continue to work closely with patients to help them recover and to prevent complications.


The psychological and emotional consequences of war, displacement and instability are still immense; the COVID-19 pandemic, with its additional burden, has only added to it. That's why mental health is a key component of many of our projects in Iraq. MSF psychiatrists, doctors, psychologists and counsellors give vital care and support to people with moderate or severe mental health issues.


As of August 2021, close to five million people have returned to their places of origin in Iraq over the last six and a half years (IOM). But nearly 1.2 million people remain internally displaced; they often lack access to adequate services, including healthcare, and water and sanitation. MSF teams have worked in displaced people’s camps and in areas where displaced people lack essential services.

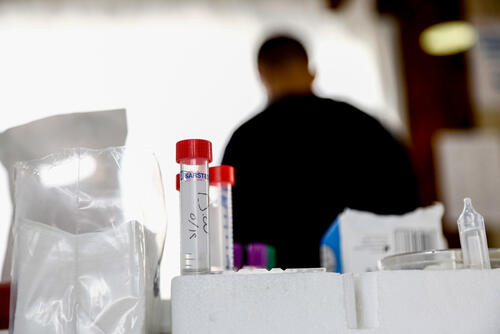
According to the World Health Organization, Iraq is among the seven countries in the eastern Mediterranean region with a high burden of tuberculosis (TB). MSF has been supporting the National Tuberculosis Programme since 2018. We aim to improve case detection, provide better tolerated and effective treatment for drug-resistant TB patients, and improving the quality of care for patients.
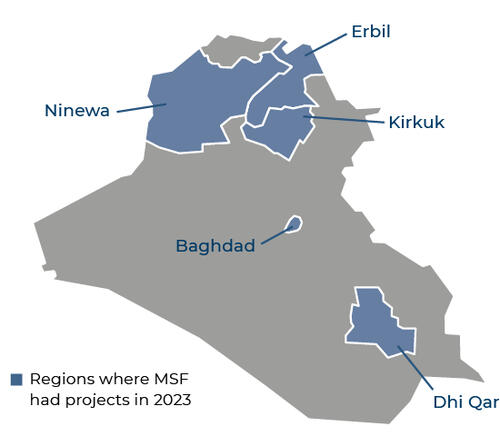
Our activities in 2023 in Iraq
Data and information from the International Activity Report 2023.
886
886
35.1 M€
35.1M
2003
2003

87,100
87,1
5,000
5,
2,830
2,83





