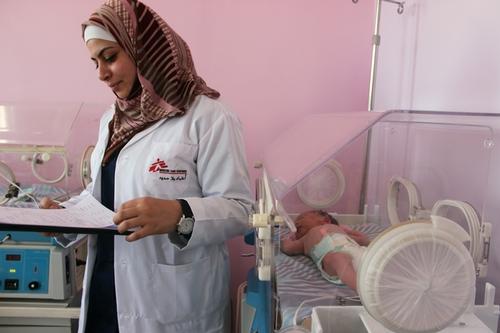
23 May marks the first International Day to End Obstetric Fistula. Here, Médecins Sans Frontières (MSF) surgeon Dr Geert Morren talks about the physical and social distress that fistulas can cause, and why the issue needs attention.
An obstetric fistula is a hole between either the bladder and vagina or the bladder and rectum, causing urine or faeces to leak continuously from the body. This kind of fistula is generally the result of a difficult birth, and can occur when pressure exerted by the baby’s head on the mother’s pelvis stops blood flowing to the tissues for too long. Often, the baby does not survive.
“For the mother, it’s a traumatising experience,” Dr Morren explains. “Not only does she go through a long and difficult birth, but she also loses the baby and ends up with a fistula that makes her incontinent.” The physical effects of a fistula often result in women being excluded from social circles. Thankfully, most cases of fistula can be treated using surgical procedures.

Fistulas are most common in places where the healthcare system functions poorly. A woman is unlikely to contract a fistula if a skilled attendant is present when she gives birth. “Fistulas are most common in places where women don’t have access to healthcare,” says Dr Morren. “We must keep in mind the social dimension of this problem: poor women are the worst affected. Some estimate that 100 to 150 women contract a fistula every day. Today, one to two million women are still in need of treatment.”
Some estimate that 100 to 150 women contract a fistula every day. Today, one to two million women are still in need of treatment.Dr Geert Morren, MSF surgeon
“Unfortunately, repairing fistulas is not a procedure that many local surgeons wish to do. First of all, it is technically quite difficult to carry out. Though it doesn’t require sophisticated equipment, it takes some time to master the technique. Secondly, it’s not well-remunerated because most of the patients are poor.”
As there will never be enough surgeons to help all fistula sufferers, preventing fistulas from occurring in the first place – by providing quality obstetric services – is key. This presents MSF with a difficult choice: should it train gynaecologists to treat fistulas, or should it focus on ensuring women have trained assistants present during childbirth? In other words, should MSF prioritise prevention? How do we resolve this dilemma?
“MSF won’t open a project that treats fistula without also investing in prevention,” says Dr Morren. “For example, in Burundi, our teams opened a specialist obstetric clinic in Kabezi and a centre for fistula treatment in Gitega. Since the beginning of the project, more than 1,000 patients have had surgery for fistula there.”
According to Dr Morren, MSF can play a lead role in training gynaecologists to treat fistulas. “We have invested a great deal in training Burundian surgeons in Gitega. If we can train enough of them to allow us to hand over the caseload and leave, we’ll call this a success.”
Urumuri health centre
In Burundi, MSF focuses on maternal health, particularly emergency obstretic care and repair of obstetric fistula. In Burundi, women are particularly affected by the lack of access to healthcare. According to the World Health Organization, 4000 of them die in childbirth each year and about 1,200 develop obstetric fistula.
In the Urumuri health centre in Gitega, central Burundi, MSF provides free care 24 hours a day to women with obstetric fistula.
In 2012, MSF surgeons performed more than 300 fistula repairs and began training two Burundian doctors to perform this operation.