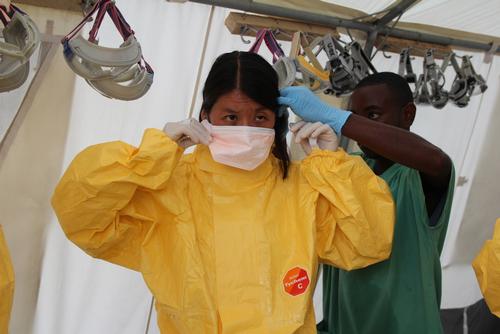
Speech delivered by Dr Joanne Liu, MSF International President
Palais des Nations, MSF side event 6pm, 20 May 2015
The Ebola epidemic in West Africa is one of MSF’s biggest emergency operations in our 44-year history. We launched an unprecedented response to an exceptional outbreak. MSF teams have treated more than 5,000 Ebola patients, one-third of all the confirmed Ebola cases reported by the WHO.
Today the Ebola epidemic is not yet over. New cases continue to fluctuate week by week in the region. With just one case, the outbreak goes on. We must double our efforts to cross the finish line.
The Ebola epidemic exposed the ugly reality of how inefficient and slow health and aid systems are to respond to emergencies. Shouts of reform have begun to echo through the hallways of power, but will it translate into real action? Will the WHO show the global health leadership that we need on the ground in emergencies?
But without strong political will of the Member States, the WHO will not reform, nor have the power and authority to function as the global health leader it ought to be. And without this, any reform will die on paper. It is time to strike the iron while it is hot, while the nightmare of Ebola is still burned into the minds of those who have lived it. Today’s momentum cannot be lost.
It is clear we are all woefully unprepared for mass disease epidemics. Countries have little incentive to ring the alarm bell and declare and respond to outbreaks, for fear of disrupting trade and harming their economies. Countries declaring and fighting an epidemic must find encouragement in the system, not economic and political punishment.
Emergency response reform is about treating people, not just global health security or strengthening health systems. Member States with the means to respond to deadly disease outbreaks in other countries cannot act only in their national self-interests, closing their borders and hoping it will burn out. They must quickly deploy resources to combat the disease at its source, to save lives and prevent further spread. Communities infected with a highly contagious virus are not biohazards. They are patients with families.
The current research and development system failed these patients in the Ebola outbreak. Biomedical innovation based on the needs of patients is required, not driven by fear of bioterrorism and defense agendas. Outcomes of R&D should be made available, affordable and accessible to those in need.
Ultimately health is a public good and therefore should remain a shared public responsibility. States must remain fully responsible for the health of their citizens and be held accountable to them.
The success of WHO reform will not be measured by the millions of dollars pledged today or speeches declaring ‘never again.’ We have heard this feel-good rhetoric before and these words alone do not save lives.
We will know if the reform has truly worked when patients on the ground directly feel its benefits - when competent people with enough resources are deployed early on an emergency with saving lives as their sole objective, leaving politics aside in favour of health. Will a cultural shift within the WHO happen, putting the humanitarian imperative of saving lives at its core in emergencies?
We, as physicians, must become allies fighting for the health of our patients. My plea, from one doctor to another: Member States, step up to the plate and assume your political responsibility. Money and words alone will not save lives without political will behind them.
We did not respond timely but we must reform truly. We cannot fail twice. Too many lives are at stake.