- The conflict between the Nigerian military and armed opposition groups known as Boko Haram has been ongoing for more than eight years, with serious humanitarian consequences.
- Aid needs to be sustained and increased, as hundreds of thousands of people remain heavily dependent on it for their survival.
According to OCHA, more than 1.7 million people are internally displaced in Nigeria's northeastern states, Borno, Adamawa and Yobe. Of these, 78 per cent are in Borno.
Over the past year, the provision of humanitarian assistance has improved but, overall, it remains inadequate, as security and access hamper the delivery of aid in some areas.
Hundreds of thousands of people depend on aid for their survival. In some places, people have been stranded for over two years, with little prospect of returning home. Needs are particularly acute in isolated enclaves outside the state capital, Maiduguri. Any disruption to the provision of this assistance could have deadly implications.
We have expanded our operations in accessible areas of Borno state that are heavily controlled by the military. There are other parts of the state, under the control of armed opposition groups, which we have not been able to reach. We have little information about the needs in these places but hear from people who have recently left that limited medical care is available. As a medical humanitarian organisation, MSF is deeply concerned about the people living in these places.
Refugees from camps in neighbouring Cameroon and people from across Borno state continue to arrive – not always by choice – in towns controlled by the military. Many of these towns are already overstretched in terms of basic amenities. Aid must be scaled up in these places, to prevent health risks to new arrivals and existing populations.
MSF medical priorities and responses
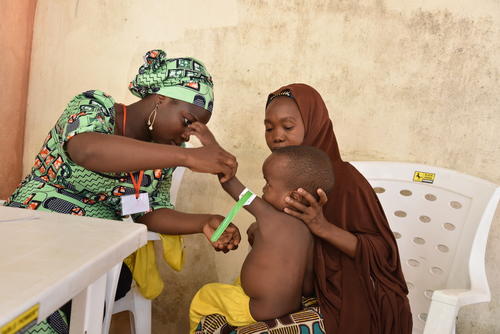
We are providing medical care to vulnerable groups, including women during pregnancy and childbirth. Our teams are running nutrition programmes for children, providing mental health support, responding to disease outbreaks and providing emergency paediatric care.
The nutritional situation has generally stabilised in Maiduguri due to a massive deployment of aid, but vulnerable pockets remain.
Access to adequate nutrition is more precarious in isolated enclaves such as Pulka, Banki, Bama, Dikwa and Rann. Freedom of movement is restricted, so people are unable to farm or fish, making them heavily dependent on humanitarian assistance. MSF provides medical aid in these locations, either through permanent health facilities or frequent visits by dedicated emergency teams.
Since August 2017, we have responded to a cholera outbreak in Maiduguri, Monguno and Mafa. This and outbreaks of hepatitis E elsewhere in the state exposed gaps in water and sanitation provision. Urgent action needs to be taken to maintain and expand existing infrastructure, especially in camps for displaced people.
MSF operations
Maiduguri is the capital of Borno state and home to around two million people, one million of whom are internally displaced, having fled other parts of the northeastern Nigerian state. The vast majority (90 per cent) live with the city’s original population, with the remainder living in official and unofficial camps around the city.
MSF operations in Maiduguri focus on maternal and child health, including nutrition, and conducting surveillance activities to ensure food, shelter, water and medical care. In preparation for the rainy season, MSF provided malaria prevention doses for children under five, as well as for pregnant and breastfeeding women.
Cholera response
Since August, MSF has been responding to a cholera outbreak in Maiduguri and Monguno and preparing to tackle any spread of the infection in other parts of Borno. Until November, we operated two cholera treatment centres (CTCs) in Maiduguri and one in Monguno, treating a total of 3,253 patients. Teams established two oral rehydration points in two camps in Maiduguri. In Mafa, we opened a four-bed cholera treatment unit (CTU) and treated 20 patients, while continuing to undertake water and sanitation activities. We have now ended our cholera treatment activities in Borno state, where the government is soon expected to declare the end of the outbreak.
Therapeutic feeding centres in Fori and Dala
MSF runs a 100-bed inpatient therapeutic feeding centre (ITFC) in Fori, a southern district of Maiduguri. The centre, which opened in January, currently treats between 70 and 80 severely malnourished children, often with complications, each week, and has a high bed occupancy rate. We also run an outpatient feeding centre in Fori for less severe cases. More than 2,000 children are currently enrolled. This programme saw 1,292 admissions from January to September 2017.
A second outpatient feeding centre in Dala, set up in anticipation of more children needing treatment throughout the summer (the traditional hunger gap period), was handed over to Terre des Hommes in September. Around 900 children were enrolled in the programme until the end of August and more complicated cases were referred to the Fori ITFC. The outpatient feeding centres in Dala and Fori have seen 5,021 admissions since the beginning of the year. MSF also began operating a cholera treatment centre (CTC) in Dala. This 80-bed CTC saw 531 admissions before its closure in September.
Borno Emergency Support Team (BEST)
BEST is a dedicated team that monitors and responds to healthcare needs across Borno state. These measures include targeted vaccination campaigns, survey coverage, nutritional screenings, distribution of therapeutic and non-therapeutic food, malaria prevention doses – known as Seasonal Malaria Chemoprevention (SMC) – medical consultations, outbreak response, and water and sanitation interventions. BEST manages interventions in camps for displaced people in Bama, Dikwa, Gajiganna and Maiduguri, as well as screening points and settlements in Maiduguri and other parts of Borno. In the months of August and September 2017, BEST was involved in the scale-up of cholera activities until the arrival of a dedicated cholera response team.
Maiduguri
In Maiduguri, we are scaling down and rationalising our activities as the situation is stabilising. In Gwange, the outpatient feeding centre has been handed over to the Ministry of Health and children enrolled in the outpatient feeding programme are referred to our centre in Fori, which has increased its capacity. In Gwange, we now focus on secondary paediatric healthcare. We are running an 88-bed paediatric inpatient department with an intensive care unit for children up to the age of 15. The capacity and occupancy rate have recently increased with the peak in malaria cases following the rainy season.
We’ve handed over its Maimusari health facility, which included a maternity ward, outpatient department and an outpatient therapeutic feeding centre, to the Ministry of Health. A paediatric outpatient department, an outpatient feeding centre and an emergency room will continue to operate in Bolori, until a handover at the end of 2017. Between the beginning of the year and September 2017, 100,332 consultations were carried out in the two paediatric centres in Maimusari and Bolori.
Since January, 11,588 malnourished children have been admitted in the outpatient nutritional programme, with an average of 297 admissions per week. Antenatal consultations totalled 41,803, while 5,697 deliveries were assisted.
In August and September, a dedicated cholera response team managed two oral rehydration points and a 100-bed CTC. As of November 2017, the cholera treatment centre at Muna (later moved to Bolori) has admitted 1,110 patients. We have now wound down all our cholera activities as patient numbers have dropped considerably.
Monguno
According to the IOM, displaced people in Monguno comprise over 122,000 who fled conflict from other LGAs in Monguno and are unable to return to their homes. The majority of internally displaced people live in four camps. Others are in non-registered sites or the host community.
MSF is the only organisation that provides secondary paediatric healthcare in Monguno, where we recorded 6,049 emergency consultations and 2,684 children were admitted to the inpatient department until September. MSF also operates an outpatient department for adults and children from camps and villages outside Monguno. A total of 34,623 consultations were carried between January and September, accounting for 25 per cent of all outpatient department consultations for OCP operated facilities in Borno state. MSF opened a cholera treatment centre (CTC) and two oral rehydration points in September to manage the cholera cases. In Monguno, MSF established the only CTC in the town and treated 1,612 until the end of November 2017.
Bama
Bama is a local government area in Borno state and is completely under the guard of the military and Civilian Joint Task Force (CJTF). According to IOM, the estimated number of internally displaced persons in Bama LGA is approximately 56,000. They are completely dependent on humanitarian assistance for survival. BEST reduced its interventions in Bama as other organisations stepped in to provide food and medical aid. This year, the team improved water and sanitation activities in January, distributed food in February and provided malaria prevention doses (referred to as SMCs) for 4,671 children under the age of five in July. A second round of SMC covered 4,567 children in August. BEST also conducted mobile clinics and nutritional screenings in Bama.
Dikwa
Most of Dikwa town has been destroyed and the population of 120,000 lives in a military controlled enclave. The entire population – which includes approximately 75,000 internally displaced people according to the International Organization of Migration (IOM) – is completely dependent on food distributions. BEST regularly visits Dikwa to provide emergency support. This includes monitoring outbreaks of diseases such as cholera, distributing food (January), and running mobile clinics (April and May). In addition, 45,456 people (aged between one and 29) were vaccinated for meningitis and 3,553 children were immunised against measles. In June, BEST supported the primary health centre and improved water and sanitation conditions in Dikwa. MSF conducted additional activities in Dikwa in October.
Ngala
The town was retaken from Boko Haram by the Nigerian armed forces in February 2015. According to the IOM, approximately 44,000 internally displaced people live in Ngala. The military is in charge of the security of the camp, but a token system allows people to leave the camp during the day. When MSF started working in Ngala in September 2016, we found an alarming situation in which access to food, water, shelter and medical care was extremely limited. This situation has considerably improved and, since February 2017, MSF has a permanent team in Ngala.
MSF runs a 54-bed inpatient department which includes maternity, delivery and neonatal care services. Teams also provide primary healthcare, blood bank services, support for victims of sexual and gender-based violence, nutritional care and outpatient consultations. The living conditions in the camp are poor. As a result, we are treating patients for illnesses such as hepatitis E. MSF has admitted 41 patients suffering from hepatitis E in Ngala since an outbreak of the disease was declared this summer. From January to September, MSF provided 19,953 outpatient consultations, 1,254 inpatient admissions, with 6,213 patients enrolled in our therapeutic feeding programmes.

Rann
Rann was attacked and destroyed by Boko Haram in 2015, which led to the town’s population fleeing to other towns in Borno and to neighbouring Cameroon. Rann was recaptured by the Nigerian armed forces in March 2016, and people started returning in April 2016. According to OCHA, around 50,000 people currently live in Rann. The population has doubled since April as people have fled ongoing military activity in the surrounding areas. MSF was providing medical care in Rann in January this year when the town was bombed, killing 100 people and injuring around 150. The Nigerian military later claimed responsibility for the bombing, saying it was a mistake. Three staff working for an organisation subcontracted by MSF were among the dead.
Following the Rann bombing, MSF mobile teams delivered medical care in Rann on a regular basis. Since September, MSF has had a permanent medical team in Rann and is now the main health provider in the town. The humanitarian situation in Rann is worrying, as the town was cut off from the rest of the country during the rainy season. Humanitarian assistance has been sporadic since it started. By September, MSF had conducted 2,887 outpatient consultations, and provided preventive treatment for malaria to 17,280 children.
Banki
People who fled the violence between Boko Haram and the military, now reside in the camp and main town in Banki. It under the control of the military and people can leave only to collect firewood in organised groups supervised by the military.
Most of the town’s original population fled in 2015 after it was taken by Boko Haram, with many crossing the border into Cameroon. The number of Nigerians returning from Cameroon, some by force, has risen over the the past months. In May alone, 12,000 people arrived. MSF started working in Banki in July 2016, after finding an extreme humanitarian situation with health and nutrition indicators far beyond emergency standards. We provided emergency medical care, screened children for malnutrition, distributed food and worked to improve the water supply.
In March, as the situation population stabilised, we handed over our medical activities to UNICEF, but continued water and sanitation support on flash visits for several days per month. During the rainy season, from July to September, we distributed mosquito nets and conducted malaria prevention activities for 33,200 children under five.
Damasak
In November 2014, armed opposition groups attacked Damasak, forcing residents to flee to neighbouring Niger and other areas in Borno state. The Nigerian armed forces recaptured Damasak in July 2016 and people started returning. MSF began providing medical care in Damasak in April, with a mass nutritional screening of 5,986 children between the ages of six and 59 months. Teams also provided care for 884 children with severe and moderate acute malnutrition, vaccinated 8,700 children (aged between six months and 15 years) for measles, and immunised 11,219 people for meningitis. We also led the medical response to the hepatitis E outbreak, referring complicated cases to MSF hospitals in Niger. To prevent the spread of malaria during the rainy season, 28,241 children under five received four rounds of preventive malaria treatment.
Damaturu
Damaturu is a town in Yobe, a state bordering Borno. Although it is relatively stable, it is always under threat from Boko Haram. People in Damaturu have freedom to move and farm with accessible markets. The main healthcare needs are malaria and malnutrition. In Damaturu Hospital, MSF operates a 25-bed emergency paediatric unit and a 50-bed stabilisation centre that treats children under five who have severe malnourishment with medication complications. From January to September, we admitted 1,235 patients to our inpatient department, conducted 33,469 outpatient department consultations, 4,122 maternal healthcare consultations, 601 deliveries, and 4,430 admissions to therapeutic feeding programmes.
In Kukerita, we run an outreach health centre and provide comprehensive primary healthcare, including outpatient department, emergency room, observation room, vaccination, antenatal care and deliveries. Patients requiring referrals are moved from Kukerita to Damaturu hospital but movement remains challenging. In Jakusko, MSF supports secondary healthcare ranging from emergency to inpatient department services. Teams screen nutritional levels and conduct referrals, epidemiological surveillance and health promotion activities among the local community.
Benisheikh
Benisheikh is a relatively stable town and home to around 28,000 displaced people. People are free to move and markets are open. Given the relative stability of the area, we have handed over our operations in Benisheikh to the Ministry of Health and various partners.
In Benisheikh until September 2017, MSF operated therapeutic feeding centres and supported a paediatric inpatient department. We also provided sexual and reproductive health and monitors health indicators in the community. From January to September, we undertook 800 inpatient department admissions, 3,152 antenatal consultations – with 261 deliveries – and 6,566 outpatient department consultations. The number of enrolments to the therapeutic feeding programmes totalled 3,200 patients during this period. We continue to provide water and sanitation services in some of the city’s camps.
In two nearby locations, MSF supports another therapeutic feeding centre in Ngamdu, and provides outpatient department care for all age groups and an outpatient feeding programme in Mainok.
Gwoza
Gwoza is heavily controlled by the military and surrounded on one side by the Sambisa forest and on the other by mountains. Both are said to be places where Boko Haram is active. The town often receives arrivals of displaced people from other areas and from Cameroon. Gwoza is only accessible by helicopter or by road accompanied by military escort.
In recent months, more organisations have joined MSF in Gwoza. To avoid duplication, we have handed over some activities while continuing to provide emergency room, nutritional care, inpatient care and sexual reproductive health services. Figures from January to September include 1,596 inpatient department admissions, 16,554 outpatient department consultations and 3,233 antenatal care consultations, with 571 deliveries. 577 children were enrolled into the outpatient therapeutic feeding programme and 141 children were admitted to the stabilisation centre.
Pulka
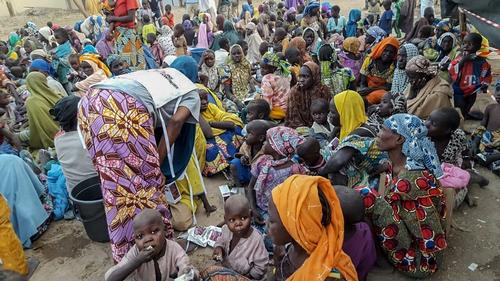
According to OCHA, Pulka town hosts 27,529 internally displaced people in the camps and the host community. The town is heavily controlled by the military, which allows people to go a short distance beyond the town’s perimeter in order to farm. Many don’t feel safe to do so. Pulka witnesses a regular influx of people because of its proximity to the border. Movement from Cameroon organised by the Nigerian military is “sometimes by choice and sometimes by force”. As a result of the unplanned and large-scale movement, shelter is lacking in Pulka. More than 25 per cent of IDPs do not have shelters, according to an IOM estimate at the end of August 2017. New arrivals in Pulka are vaccinated and provided non-food items like jerry cans and mosquito nets, and children undergo nutritional screenings.
MSF provides primary and secondary healthcare including outpatient care, emergency room, ante- and postnatal care, and referral services. We also run mental health activities, community surveillance, and water and sanitation services for people living in the hospital grounds. From the start of the year until September, we admitted 1,536 patients to inpatient department care, carried out 24,749 outpatient consultations and conducted 3,588 antenatal care consultations (with 601 deliveries). During this period, 1,072 children were admitted to therapeutic feeding programmes. We also put in place an emergency team to tackle malaria and cholera.
Mafa
In response to the cholera outbreak, we continue to undertake water and sanitation activities, including the construction of showers, latrines and a borehole in Mafa.




