Anthropologist Roberto Wright is working in Ethiopia’s Somali region to help MSF reach and be accepted by local communities.

It’s 8am in Galorgube, a small town in Doolo zone in the Somali region of Ethiopia. The sun is already strong. Until late 2016, this area was greener and less populated than it is today. But, after a series of failed rainy seasons, the ground turned orange and became dotted with hundreds of tents. They belong to the nomadic pastoralist people who were forced to settle here after the drought killed the animals on which they depend.
In a dark tent, a tall, bearded man in an MSF T-shirt and his patient translator have spent an hour talking with a group of about 40 men ─ mostly elders ─ who represent this community. The tall man is Roberto Wright, from Brazil, MSF’s anthropologist in the emergency team. He has been working in the Somali region since the end of June.
“We found a compromise that respects their perspective and, at the same time, upholds our medical objectives,” says Roberto, when he finally leaves the tent with a big smile on his face. The community leaders have just agreed that a severely malnourished child can be transported to be treated in the inpatient treatment feed centre in Yucub, just six kilometres from Galorgube. They had previously refused, preferring the services of their traditional healers.
“Part of my work is to understand their approaches regarding traditional medicine and to explain MSF care to them so that they can combine both,” says Roberto. “If they don’t understand what MSF does, they will never seek our services or come to our health centres.”
To achieve that goal, Roberto trains and works alongside hundreds of hardworking health workers, most of them either locals or displaced pastoralists. Every morning, they divide into pairs and spend the day talking with the displaced people, particularly the women, most of whom have between three and eight children. The health workers ask questions to discover if any of their children have severe acute malnutrition or other complications that need medical treatment. With the shortage of food in this area, the teams have been sending an average of 10 children per week to MSF’s health facilities for treatment.

Seeking acceptance
“We need to adjust the way we work to their perspective, in order to fit in with their community practices,” says Roberto. His main goals in the Somali region are to help MSF reach these communities and be accepted by them. He has carried out similar work in Iraq, Sierra Leone, Central African Republic and Turkey, but here in Ethiopia, it requires spending much more time in the car. Distances in the Somali region are huge, and the various communities are far from each other. In two months, Roberto has spent 60 days non-stop on the road and covered more than 6,000 kilometres.
Today he drives from Yucub back to Galorgube to transport a one-year-old baby to MSF’s health facility. The baby’s mother and the community elders have agreed that MSF should treat him. From Galorgube, he will be transferred to the MSF-supported Wardher hospital, an hour’s drive away.
The baby’s mother is 25 years old, has four older children and is two months’ pregnant.
“We were living in the bush with 200 animals,” she says, “But now we only have 10. They all died. This is my younger child and he has been sick three times already.”
A new type of crisis
Before going to Wardher, Roberto and the outreach team will drive in a convoy for two more hours to Lahelow, a settlement for displaced people in a remote dry area. They will visit the mobile nutritional clinic, where Roberto will meet the MSF team to find out how people in the camp are surviving.
“For me, the challenge in the Somali region, apart from the long distances, is to understand how people are trying to adapt,” he says “They are used to crises but, in this one, their livestock are dying so fast, which is something they’ve never seen before. They need a platform to exchange ideas to work out what to do next. We want to develop this at the community level but also inside the heath facility in a health promotion tent.”
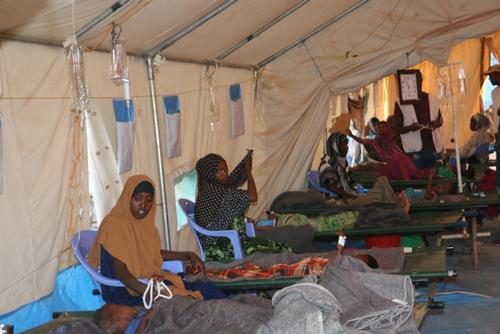
After another 65 kilometres, the car arrives at Wardher hospital, where there are six tents and two wards for malnourished children.
The key to providing medical care
The sick baby and his mother are taken by nurses to the waiting area, while Roberto jumps out to see how the new ward is going. Later, he recalls the night an MSF doctor called him because a mother wanted to leave the hospital with an unconscious child and go to the traditional healer.
“That evening I went to the hospital to talk to the mother, find out why she wanted to leave and try to find some common ground,” says Roberto.
“When I asked why she wanted to leave the hospital, she said: ‘I want to give my child traditional treatment. She must be exorcized. I want a sheikh to read the Quran to my child.’ I replied, ‘That is something we can help with.’”
As part of his community engagement strategy, Roberto had already engaged with key religious leaders, so he called a sheikh to go there. The evening finished under the stars, with a soft voice reading the Quran and the baby being cared for in the hospital.
It may not be a classic MSF role, but Roberto’s job as an anthropologist is an important part of the chain. He listens to local people and tries to understand them. And this, in the Somali region, has proven to be key to MSF’s ability to provide medical care.