Summary
Since the Ebola epidemic in Democratic Republic of Congo (DRC) was declared on 8 May 2018, over 60 people who presented symptoms of haemorrhagic fever, including 38 confirmed Ebola cases and 28 deaths (of whom 14 were confirmed as Ebola)Latest figures (source: DRC Ministry of Health) – date of info: 19 June 2018, have been notified by the national health authorities in the Equateur region, in the west of the country, where the outbreak started. 24 patients (confirmed Ebola cases) have recovered from the disease and been discharged from treatment centres.
| Suspect cases | Probable cases | Laboratory-confirmed cases | Deaths among confirmed patients | Total deaths | |
|---|---|---|---|---|---|
| Mbandaka Health Zone | 0 | 0 | 4 | 3 | 3 |
| Bikoro Health Zone | 4 | 11 | 10 | 7 | 18 |
| Iboko Health Zone (including Itipo) | 4 | 3 | 24 | 4 | 7 |
| Ingende Health Zone | 2 | 0 | 0 | 0 | 0 |
| TOTAL | 10 | 14 | 38 | 14 | 28 |

5 things to know about the Ebola vaccination
Current situation
So far, the outbreak has affected the health zones of Bikoro (Bikoro and Ikoko villages) and Iboko (Itipo and Iboko villages), with four laboratory-confirmed cases of Ebola also detected in the city of Mbandaka, the main city of the region. Two suspected cases have been recorded in the Ingende health zone. As of 19 June, there had been no Ebola-positive patients under treatment in DRC for a week, but hundreds of contacts remain under surveillance and areas of uncertainty remain in some villages.
This is the ninth Ebola outbreak in DRC in the last 40 yearsPrevious outbreaks in DRC: Yambuku (1976) 318 cases - 280 deaths; Tandala (1977) 1 case -1 death; Kikiwit (1995) 315 cases- 250 deaths; Mweca (2007) 264 cases - 187 deaths; 2008-2009- 32 cases - 15 deaths; Isiro (2012) 36 cases - 13 deaths; Djera-Boende (2014) 66 cases - 49 deaths; Likati (2017) 8 cases - 4 deaths (source: DRC Ministry of Health) . So far, most of the previous outbreaks have occurred in relatively remote and isolated areas, with little spread of the disease. The last Ebola outbreaks in DRC occurred in Likati district in May 2017, with eight people infected, of whom four died, and in Boende (Thsuapa region) in 2014, with 66 people infected, of whom 49 died.
Unlike in previous Ebola outbreaks in DRC, where most of the cases have been concentrated in remote villages, this time patients have also been diagnosed in Mbandaka, a Congo River port city of more than one million inhabitants. While easy access to transport increases the risk of the virus spreading, surveillance is being reinforced. Despite the media hype, it is important to emphasise that the epidemic has not spread widely within the city.
During the past few weeks, MSF has been working closely with the Congolese Ministry of Health (MoH) and with other organisations on the ground to coordinate the response.
The response is based on the ‘six pillars’ of Ebola intervention:
- Care of diagnosed patients and isolation;
- Outreach activities to find patients;
- Tracing and follow-up with patient contacts;
- Health promotion activities to inform people about the risks and how to avoid them;
- Support of regular primary healthcare;
- Safe burials to avoid infections.
If this intervention is followed well, an Ebola epidemic can often be contained in a relatively short period of time.
For all these activities, building a good understanding with local communities is vital. Medical and health promotion teams are working hard to explain to the population what the symptoms of Ebola are, how to avoid contamination, the importance of coming to health structures as quickly as possible if they suffer from symptoms, and the importance of isolation measures to contain the disease. The sooner patients are admitted and receive medical care, the sooner their families are protected and the greater the chance of limiting the spread of the epidemic.
After almost a month since the outbreak was officially declared, the epidemiological picture is beginning to clear but areas of uncertainty remain. Now is certainly not the time for complacency, the six pillars of the Ebola response must be meticulously implemented and maintained, with a particular focus on outreach and surveillance activities, in order to end this outbreak.
Staff on the ground, 19 June 2018
Currently there are 470 people working in the field on the MSF Ebola response in DRC, the vast majority are Congolese and from the affected region.
Supply material, 5 June 2018
Supply material includes:
- medical kits
- protection and disinfection kits (isolation items such as gloves, boots and Personal Protective Equipment-PPE, etc.)
- logistic and hygiene kits (plastic sheets, jerry cans, water distribution kits, chlorine spray kits, water treatment kits, etc.)
- drugs
- transport (cars and motorbikes)
- tents and construction material for building ETCs
As part of MSF’s emergency preparedness in DRC, some supplies were already available in Kinshasa. These were sent to hotspot zones as soon as the outbreak started.
Almost 100 tonnes of supplies (sent from MSF supply centres in Europe) have been received in Kinshasa, and an additional 15 are expected by the end of the week. A total 63 tonnes of supplies (medical and logistical supplies, including six vehicles and 10 motorbikes) have already been sent to Mbandaka and Bikoro, with more to be sent in the coming days.
Activities
MSF’s Ebola response in DRC started on 5 May, with an epidemiological alert in the Equateur region. A small team from MSF’s Congo Emergency Pool (PUC) assessed the situation, together with teams from the MoH and WHO. When the Ebola epidemic was officially declared on 8 May, experts from MSF’s emergency pools arrived in the field to deploy a rapid response in the Ebola hotspots. Among the MSF staff on the ground are some our most experienced Ebola field workers, including medical personnel, experts in infection control and logisticians.
Mbandaka
An MSF ETC with 12 beds has been operational in Mbandaka since 28 May. In addition to the treatment and isolation of suspected and confirmed Ebola cases, the focus of MSF’s response is on surveillance, investigation of new cases and their contacts, infection control and prevention, health promotion, safe burials and training activities with the MoH staff. Plans for the handover of these activities are under way and will be shared in the coming weeks.
Bikoro
In Bikoro, MSF has set up an ETC with 20 beds in partnership with the MOH, and continues to reinforce outreach activities including case investigation, monitoring and surveillance. There are also two teams who respond to alerts about suspect and probable cases in the surrounding villages. These activities will be progressively handed over to the MoH and other actors in the coming weeks.
MSF has recently helped to set up a survivor clinic to take care of post Ebola complications and mental health issues amongst those who recovered from Ebola. The clinic will be run by an MoH doctor.
Kinkole – Kinshasa
Construction of a 10-bed (extendable to 40) ETC at Kinkole (Kinshasa suburbs) is finished. MSF staff have been carrying out training (on protection measures, treatment procedures, and transport of patients) to MoH and DPS (provincial health authorities – Département Provinciale de la Santé) staff, who will manage the structure in case of need.
Itipo
ALIMA has finished constructing their Ebola Treatment Centre in Itipo so MSF will close the 14-bed transit centre on 20 June. All future suspect and confirmed cases in Itipo will be cared for by ALIMA and not transferred to MSF in Bikoro. Some of the MSF team from Itipo will finish their mission whilst others will be redeployed to support MSF’s teams in Iboko.
MSF is also currently working to set up a survivor clinic in Itipo (the epicentre of the outbreak and the home of most of the survivors) alongside the MoH and ALIMA.
Iboko
MSF continues to run a 13-bed ETC in the Iboko General Reference Hospital in partnership with the MoH. In addition, MSF teams are also assisting with other areas of the Ebola response, including ambulance services, contact tracing, active cases finding, health structure support, health promotion, safe burial and the disinfection of health centres and houses. MSF is also supporting the paediatric department of the Iboko General Reference Hospital with non-Ebola health care and working alongside MoH staff to improve infection prevention and control in the hospital.
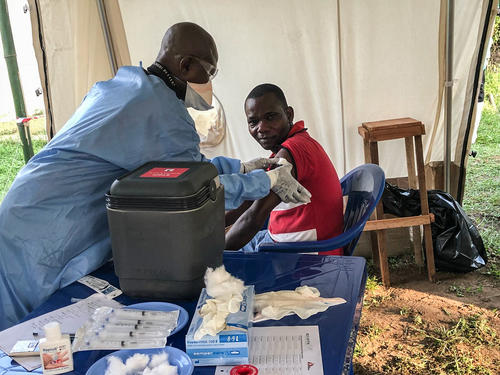
Vaccination
MSF and our epidemiological research unit, Epicentre, are working with the local health authorities and the World Health Organization (WHO) in the use of the Ebola vaccine rVSVDG-ZEBOV-GP, which is being used as part of the overall strategy to control the Ebola outbreak.
MSF’s vaccination activities started on 28 May and have targeted villages and towns in the Bikoro and Iboko health zones, including Itipo, the area most affected by the outbreak. The vaccination has been administered according to a ring approach (targeting contacts and contacts of contacts of confirmed Ebola cases) as well as frontline workers like health workers and hygienists working in Ebola Treatment Centres, religious leaders, traditional healers and moto taxi drivers.
As of 17 June, 1,436 people have been vaccinated by MSF. If there are no new cases, vaccination activities will soon finish, and the teams will be purely focused on follow up.
The vaccinations are voluntary and free-of-charge. This vaccine has not yet been licensed and is therefore being implemented through a study protocol, which has been accepted by the national authorities and the ethical review board in Kinshasa, as well as MSF’s ethical review board.



