Discover all our latest news, stories and publications. Use the filter to get to the content you're looking for.

Nasser hospital, southern Gaza’s last lifeline, must be preserved

People killed and injured by landmines in Deir ez-Zor as they return home

MSF report reveals stark lack of protection and assistance in South Darfur, Sudan

Voices from South Darfur

Yemen: MSF hands over activities in Marib and Taiz city to local authorities

MSF calls for urgent aid to support Sudanese refugees fleeing to Chad

Dozens of Palestinians massacred at US-Israel backed food distribution sites

In Gaza, disastrous food distribution “confirmed that the US-Israel plan to instrumentalise aid is ineffective”
MSF closes day care centre in Athens after nine years of providing care

Sexual violence in Sudan: “They beat us and they raped us right there on the road in public”

Displacement orders are “psychological and physical warfare” in Israel's campaign of ethnic cleansing in Gaza
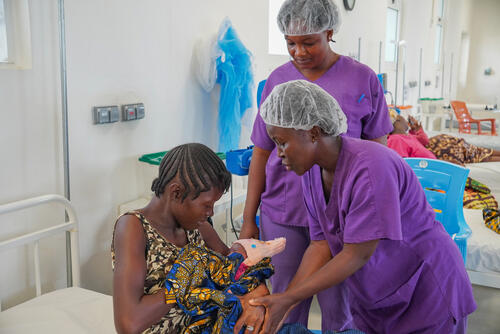
Complementing the knowledge and skills of the medical staff in Sierra Leone

Dedicated health professionals improve care for people on Kiribati

Additional 30,000 Rohingya to receive hepatitis C treatment in Cox’s Bazar
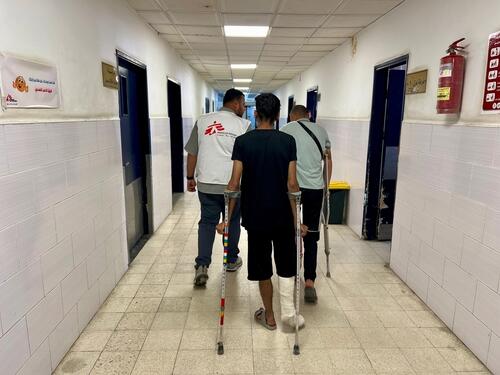
Aid instrumentalised, health system under fire: Gaza is being deliberately asphyxiated by Israeli forces

Deadly Gaps: Don't turn away from saving lives

UK government must immediately close Wethersfield mass containment site for asylum seekers

MSF denounces deliberate humanitarian catastrophe caused by siege on Gaza

Increase in admissions at MSF centre specialised in treating people for extreme violence in Mexico City

Response to devastating earthquake in Myanmar driven by solidarity and dedication

Sudan: MSF returns to Khartoum’s Bashair Teaching hospital amidst soaring cholera needs

People fleeing Zamzam camp arrive to overwhelmed humanitarian response in Tawila

Burundi: Congolese refugees in Musenyi site face humanitarian and health emergency

South Sudan: MSF strongly condemns the deliberate bombing of our hospital in Old Fangak, Jonglei state

How we deliver medical humanitarian assistance
Everywhere we work, the circumstances are unique. Nonetheless, our programmes generally follow a common set of practices designed to make sure our resources and expertise are used to maximum effect.



