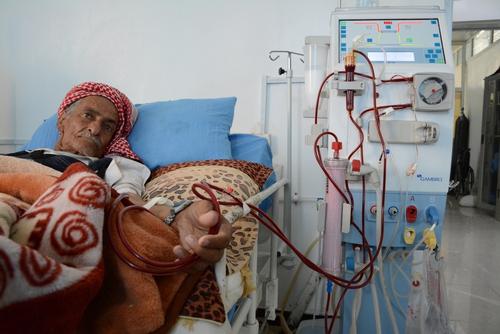
Many civilians continue to live in Saada, northern Yemen, despite almost daily airstrikes in the area. Michael Seawright from Auckland, New Zealand, was recently Project Coordinator for Médecins Sans Frontières (MSF) projects in the war-torn region.
“I’ve worked in war zones for the past 11 to 12 years, in some of the worst conflicts like Syria, but I have never seen such destruction conducted in such a short period as in Yemen. I was based in Saada, in the north, in a Houthi-controlled area that was experiencing almost daily attacks from Coalition air forces. These air strikes were often close to our facilities and we clearly felt their effects.
As Project Coordinator, an important part of my job was helping new staff acclimatise to the security situation. While most of our staff were experienced with MSF, many were yet to experience that level of conflict, and close proximity to attacks.
Extreme trauma injuries
I’d never before seen the level of casualties I saw in Saada. The scale of wounded was extreme in two respects – firstly there was a large number of wounded coming through the hospital, but second the severity of wounds was also often extreme.
MSF was running the emergency department, operating theatre, inpatient and maternity ward in what grew to become a 93-bed hospital in Saada City. We were receiving a lot of patients with severe injuries, including traumatic amputations – people would come in missing feet, hands and with severe abdominal and head trauma. Many of the wounded had travelled from four to five hours away, given that it was the only hospital with emergency surgical capacity in the province, in fact in most of northern Yemen. There were lots of patients: we were seeing over 2,000 emergency cases a month and more than 100 surgeries a week. If you combine that with the security situation keeping people awake, it was quite challenging, especially for our medical staff many of whom were on call 24-hours a day due to staff shortages across the country.
Despite the volatility of the conflict, life goes on, and as always pregnant women need somewhere safe to deliver their babies. The maternity ward, supported by MSF, delivered over 100 babies a week in the hospital. This was a source of pride for them but also reassuring for the wider population to know that while lives were being lost new life was being created.
Protecting a child
One patient whose story was particularly moving was a three-year-old boy with severe burns who came in to the emergency department in Saada with his uncle and father. The family lived near the Saudi border, in an area where there were regular indiscriminate attacks against the community. One day while their house was being hit by coalition forces, the boy’s father and uncle, in concern for their little boy, jumped on top of him to protect him. For me it highlighted that a family in Yemen is much the same as a family here in New Zealand or Australia. What father or uncle doesn’t want to protect their son or nephew? And in this case they literally put their bodies between the blast and him. Unfortunately, he was still quite burnt down one side of his body, but he will recover with no significant scarring, according to our doctors.
The little boy was one of several long-stay burns patients in our hospital. Where the injury needed further treatment and the service existed elsewhere, MSF organised and paid for all referral support – including treatment costs, transport, food and the costs of the caregiver. But some people chose to stay for a variety of reasons, such as family commitments. So we had a number of long-stay patients, particularly children.
Negotiating with authorities
Another important part of my role was negotiating with the military and local authorities. Without their permission, irrespective of what we want to do, we are simply unable to safely conduct medical activities. One thing that really helped us was the fact that our results spoke for themselves. The large number of patients that MSF was treating, combined with the number of facilities that we were supporting, allowed a significant level of access to communities requiring critical healthcare. Also the fact that MSF is privately funded allowed us a high level of operational freedom in Yemen.
Emergency care on the border
Even though our impact in Saada was very high, we were still four hours away from the Saudi Arabian border where large numbers of casualties were occurring. In order to access border communities with critical medical needs, MSF provided fuel for ambulance referral services from the border to the hospital so that the cost of fuel – which was extremely high – was not a barrier for patient care. This helped, but it was still a four hour journey over what was worse than any road I have driven in New Zealand.
In early November 2015 MSF started supporting an advanced stabilisation point – essentially an emergency room – right near the border, so that people didn’t have to travel four hours for healthcare. For critical patients, that could mean the difference between life and death. If you can stabilise patients before they’re moved then they have a much greater chance of survival. Unfortunately, while the facility had been operational for almost three months, on 10 January 2016 it was hit by a military projectile, causing several buildings to collapse. Six people were killed, including three staff, and seven people were seriously injured, including two staff.
This was another reminder that the sanctity of healthcare was no longer respected in Yemen with civilians continuing to bear the brunt of the conflict.”
MSF manages 11 hospitals and health centres and regularly supports 18 health centres across Yemen. Since the start of the current crisis in March 2015, Médecins Sans Frontières teams have treated more than 20,000 war-wounded patients.