In addition to recurrent conflicts, the country continues to suffer from concurrent emergencies, including severe flooding, food insecurity and disease outbreaks. According to the United Nations*, two-thirds of people are in need of humanitarian assistance such as food, water and healthcare.
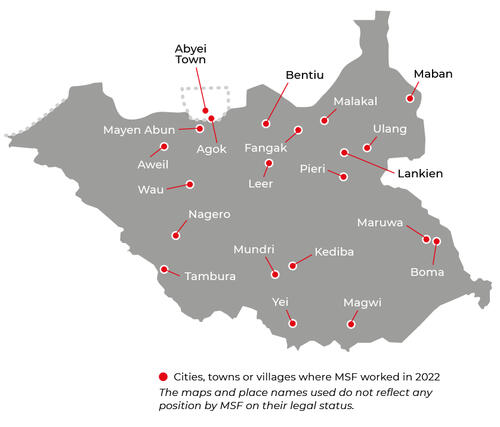
Our teams provide a range of services including general healthcare, mental healthcare and specialist hospital care. Our mobile teams also provide health assistance to displaced people and remote communities in eight of the country’s 10 states and in two administrative areas. In addition to responding to emergencies and disease outbreaks, we also carry out preventative activities, such as vaccination campaigns, seasonal malaria chemoprevention, safe drinking water and non-food items distribution.
*OCHA
Why are we here?


Tens of thousands of people in South Sudan have died and roughly one in three have been forced from their homes since renewed conflict broke out in December 2013. Our teams are constantly adapting their response to ensure we can continue providing displaced people with medical and humanitarian assistance. We also provide much-needed medical and mental healthcare in the former and current Protection of Civilians camps, where hundreds of thousands of people remain trapped in a hostile and insalubrious environment.


Medical care is practically non-existent for people living in remote areas in South Sudan. MSF runs hospitals and clinics and supports existing government-run facilities, in particular with maternal, paediatric, neonatal and surgical care, and mental health support. Our teams also train community healthcare workers and run outreach and preventative activities, such as vaccination campaigns.


South Sudan experiences recurrent infectious disease outbreaks, including measles and cholera. Malaria is also endemic and is one of the leading causes of sickness and death especially among children. In collaboration with the Ministry of Health, we organise mass vaccination campaigns against these diseases. We also provide seasonal chemoprophylaxis for malaria – and for all diseases we provide care and treatment for patients.


South Sudan has a high burden of neglected diseases such as kala azar, sleeping sickness and snakebites. Our teams provide specialised care to people suffering from these diseases in our facilities. We also advocate for better access to treatment, since very few options are available in the country.


South Sudanese have experienced successive years of flooding caused by heavy rains. Hundreds of thousands have been forced to leave their homes and live in dire conditions with limited access to healthcare, drinking water and food. This recurrent situation has amplified the risk of outbreaks of infectious and water-borne diseases. We run mobile clinics in remote areas to improve access to healthcare and often provide emergency referrals by boat. We also distribute emergency items such as tents and water containers.


Providing clean drinking water, and correctly processing wastewater, protects people from waterborne diseases such as cholera. Our teams provide clean water and run a waste management system in all the health facilities where we work. We also assist with the provision of safe water and adequate sanitation conflict-hit regions and in areas where displaced communities live.


After decades of conflict and underinvestment, the severe shortages of health infrastructure and qualified medical professionals continue to pose major challenges to the development of a good healthcare system in the country. The MSF Academy for Healthcare is training locally hired South Sudanese healthcare workers in several states to strengthen competencies and improve the quality of care.
Our activities in 2022 in South Sudan
Data and information from the International Activity Report 2022.
3,460
3,46
€112.1 M
112.1M
1983
1983

891,000
891,
309,900
309,9
125,000
125,

62,500
62,5
12,600
12,6
6,460
6,46

4,610
4,61
3,810
3,81
2,540
2,54

A year in pictures 2017

Delivering HIV treatment to conflict areas

Continuing displacement is the new reality for many along northern frontier

MSF strongly condemns the armed robbery of its clinic
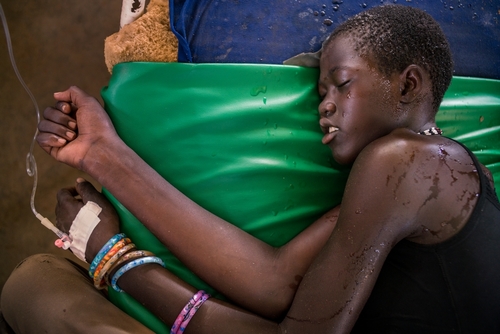
Malaria preparedness vital as rains begin

MSF urges G20 to take action on health issues

Malnutrition on the rise in Pibor

MSF welcomes WHO decision to include snakebite on Neglected Tropical Diseases list





