People’s lives in Nigeria have been disrupted by violence and crime, while regular disease outbreaks continue to endanger the lives of thousands of children.
MSF has been responding to disease outbreaks and emergency health needs in Nigeria for many years, focusing on maternal and paediatric healthcare throughout the country. Since mid-2021, we have scaled up our nutritional activities in the Northwest, as a growing yet largely ignored malnutrition crisis is pushing people to the limits.
Why are we here?


In recent years, violence and insecurity have increased humanitarian needs in Nigeria. It has been 13 years since an insurgency began in northeast Nigeria, with armed opposition groups fighting the Nigerian army. Thousands have been killed in fighting and many more by malnutrition, measles and malaria. People are unable to farm or sell their goods and mass displacement has resulted in catastrophic living conditions.
Our support for displaced people and host communities includes maternal and paediatric care, mental health support, treatment of malnutrition, support for survivors of sexual violence, provision of water and sanitation, non-food items and shelter. In providing healthcare access for refugees coming from Cameroon, we are also supporting healthcare services in Cross River state since March 2022.


Nigeria currently accounts for 10 per cent of global maternal deaths, the fourth-highest number worldwide, according to UNICEF*. Each year, approximately 262,000 babies die at birth, the world’s second highest number.
Our teams run the maternity and neonatal departments of Jahun general hospital, in Jigawa state, and support basic obstetrics in health centres to reduce complications during pregnancy. In 2021, we assisted 17,500 births. We also support maternal and child healthcare in Kano where we assisted 1,436 deliveries in the first six months of 2022.

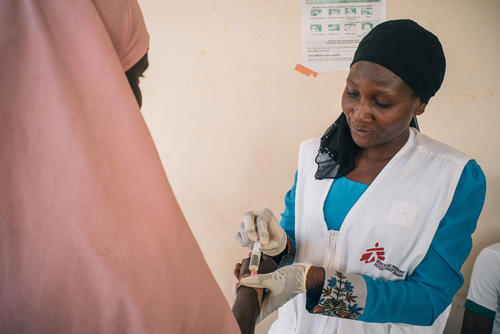
In collaboration with Nigeria’s Ministry of Health, our teams support mass vaccination campaigns carried out across the country against diseases such as measles, meningitis and pneumococcal pneumonia. We also provide seasonal malaria chemoprevention. In Ebonyi state, we support health authorities to treat Lassa fever patients through technical support and staff training at a teaching hospital in Abakaliki.


We support the Noma Children’s Hospital in Sokoto with acute medical care and reconstructive surgery for patients with noma. Most patients with noma ─ a disfiguring and often deadly infection ─ are children under six, whose immune systems have been weakened by malnutrition. In addition to surgery, our team provides physiotherapy, nutritional and mental health support, and conducts outreach activities to improve early detection. In 2021, our staff conducted 105 surgical interventions.



We run programmes for victims of sexual and gender-based violence in our projects in Benue and Zamfara. This include preventive treatment for sexually transmitted infections, emergency contraception, counselling and psychosocial support.

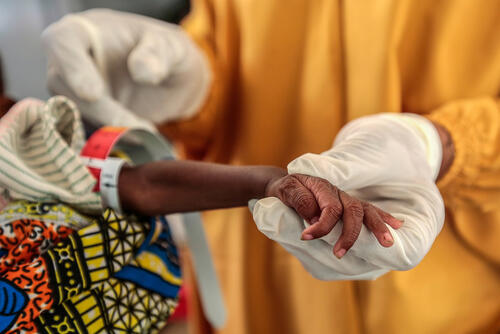
A large proportion of people in Nigeria’s Northeast and Northwest regions are chronically vulnerable to food and nutrition insecurity. A combination of factors including escalating violence and the disruption of access to farming, widespread displacement, soaring food prices, and epidemics, is driving a growing health and nutrition crisis.
MSF runs a 120-bed nutritional centre in Maiduguri in Borno state. In addition, we collaborate closely with the Ministry of Health by supporting services in 21 outpatient and eight inpatient nutrition facilities across five states in the Northwest – Zamfara, Sokoto, Katsina, Kano and Kebbi.
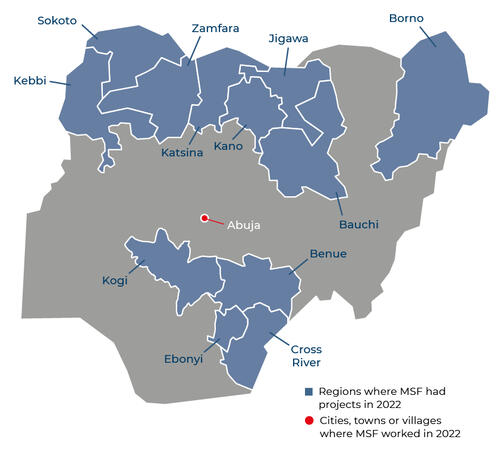
Our activities in 2022 in Nigeria
Data and information from the International Activity Report 2022.
2,830
2,83
€91 M
91M
1996
1996

945,500
945,5
348,100
348,1
185,400
185,4

116,800
116,8
36,900
36,9
25,000
25,

23,100
23,1
12,200
12,2
3,800
3,8

Surviving sexual violence in the camps of Benue

Neglected humanitarian crisis escalates in northwest Nigeria

An arduous journey for pregnant women to access healthcare in northwest Nigeria
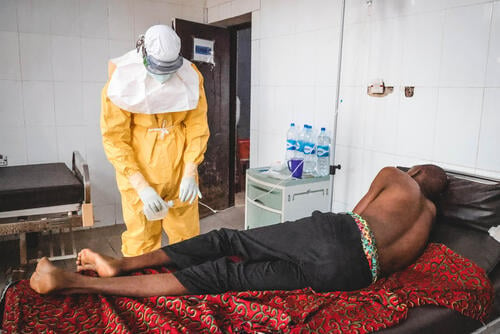
Tackling the spread of Lassa fever in Nigeria

MSF joins noma survivors in celebrating inclusion in WHO neglected tropical diseases list
Dramatic upscaling of vaccination needed in West Africa to curb deadly diphtheria outbreaks

Urgent response needed to curb Nigeria’s worsening diphtheria outbreak

Abortion: Women more at risk of death in fragile and conflict-affected settings








