Sivapalan Namasivay is an experienced anaesthesiologist. Since 2011, he has worked on several assignments with Médecins Sans Frontières (MSF): in Yemen, in Port Harcourt (Nigeria), and more recently in Syria. He has just spent a month in Jahun Hospital in the North of Nigeria, where MSF is responsible for maternity care, especially emergency obstetrics and newborn care.
What is MSF doing in its program in Jahun?
It is primarily focusing on maternal care. MSF operates out of a Government hospital facility where we are responsible for women coming in for maternity care. Pregnant mothers arrive here with serious complications such as cardiac failure secondary to severe anaemia and convulsions from severe eclampsia (high blood pressure in pregnancy). We try to reduce the associated morbidity (sickness or disease) and mortality by managing these complications and then providing a safe childbirth either by normal delivery or caesarean section. We also run a surgical treatment facility for the repair of vesico-vaginal fistulas (VVF). VVF is a terrible physical and psychological debility arising as a complication from improperly managed childbirth.
What did your mission consist of?
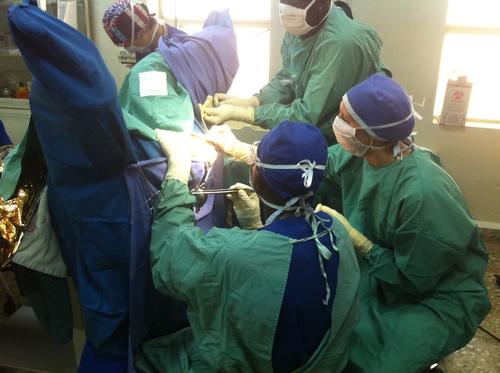
I was working in the operating theatre as a medical anaesthetist, where I supervised and assisted the three nurse-anaesthetists who provided the day to day anaesthetic services. Aside from that, and what I perceived as a more important role, was managing the medical emergencies of the patients admitted to the intensive care unit.
How important was your role in the treatment/care of our patients?
Most of our patients arrive in a compromised state of health and, what more, with the added problem of being in the late stages of pregnancy. The obstetricians work hard to ensure a safe delivery and the paediatrician takes care of the newborn. But the large majority of these patients have other complications that could endanger their lives and that of the unborn baby. In this situation, it is my role to manage these complications pre- and post-delivery and, when surgery is indicated, provide a safe mode of anaesthesia. Then there are also the patients admitted for extensive VVF repair surgery. Managing them pre-, intra- and post-surgery is also another responsibility of the medical anaesthetist.
What are the main difficulties faced by our patients?
A lot of young girls are married early, as young as 15 years old. They get pregnant at a very young age and also experience multiple pregnancies. Malnutrition and especially its associated anaemia make these pregnancies a health risk for both mother and child.
Also there is almost no ante-natal check-up. Then there is the prolonged labour they are subjected to; some are brought to the hospital after being in labour for as long as 36-48hrs. The incidence of difficult and obstructed labour is an important cause of the resultant VVF that these patients eventually suffer.
Can you share some patient stories?
A 16 year-old pregnant girl was brought to the hospital for breathing difficulties. She was found to be in cardiac failure secondary to very low haemoglobin of 2gm/dl. The normal level would be 12-15gm/dl. We managed to treat her cardiac failure and also transfuse blood to improve her haemoglobin level. Sadly the unborn foetus was diagnosed to be dead in-utero. Thus the patient had to be induced to deliver a dead baby. Apparently a year ago she had delivered a still birth.