The health risks for children are more severe the younger the child: as a global average, 85 per cent of childhood deaths occur in children less than five years old, but 47 per cent of those deaths are in the newborn period – the first 28 days of life.
Children under 15 years of age make up more than 60 per cent of patients in our projects, and many arrive in a critical condition or in the late stages of an illness. They are sick because they have not been adequately protected from disease or received appropriate treatment when they needed it. There are still many gaps in appropriate drugs, tools, protocols and staff for treating these young patients.
These are all factors why children under five in low- and middle-income countries continue to lose their lives to infectious diseases such as pneumonia, diarrhoea and malaria, and why newborns are failing to survive their first few days. This is also why older children face poor health long-term, if not death, due to chronic illnesses such as diabetes and epilepsy.

295,300
295,3
596,790
596,79
5,785,000
5,785,
Quick facts about child health


Although deaths in children aged under five are declining overall, the same cannot be said for newborns. As a result, the proportion of newborn deaths amongst under-five deaths continues to increase. The main causes of newborn death are prematurity and low birthweight, sepsis (severe general infection), and birth asphyxia (a medical condition resulting from lack of oxygen during birth). The majority of these complications are preventable or treatable, as long as they are recognised early enough by a skilled attendant who is trained to know how to respond. In MSF delivery rooms this is typically a midwife, trained in newborn resuscitation, who is able to focus on the baby but also call for additional help if needed.

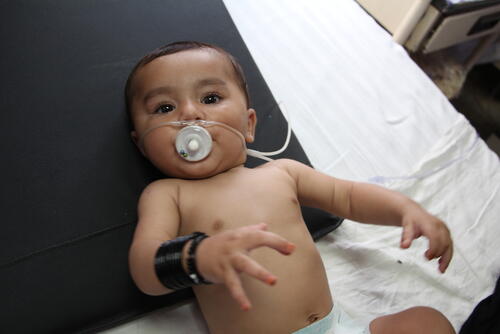
In a resource-poor setting or a sudden-onset humanitarian crisis, children are often exposed to preventable disease, due to lack of water, hygiene and access to healthcare. For children aged 1-59 months, the most deadly threats are pneumonia, diarrhoea and malaria, but these will also often complicated by malnutrition – and vice versa, in a vicious cycle. Especially in the African region, infectious diseases still account for 60 per cent of under-five deaths, many of which are vaccine-preventable. Improving child survival depends on a reliable immunisation program, but gaps remain in many countries.


Despite the risk of death decreasing in older children and young adolescents compared to under-fives, they still face concerning levels of preventable death and ill health, especially in low and middle-income countries. While infectious disease continues to play a big role, older children can be affected by chronic diseases such as diabetes, asthma and epilepsy, which they will live with for the rest of their lives. To help them manage their disease and avoid long-term complications including death, they and their families need comprehensive, long-term treatment and support, but this is often sorely lacking in resource-poor settings.


Effectively preventing, detecting and treating sickness early keeps children healthier, avoiding serious illness in most. This is only possible if healthcare is available close to where people live: in their community. One obstacle is the lack of health professionals in rural and remote settings. Community Health Workers are proving pivotal to fill that gap. With training and ongoing support, they can provide basic medical check-ups; undertake nutritional screening to identify children with acute malnutrition and dispense therapeutic food; test, diagnose and treat simple malaria, as well as distribute bednets, for example. Integrated community-based models are also key to linking children to higher level care if they do become severely ill.


Most critically ill children in low-resource settings die without having access to paediatric critical care. These are children who have succumbed to advanced stages of severe disease or acute illness complicated by other diseases or conditions. Of those critically ill children that do reach a hospital, many die within the first 24 hours. The first obstacle they face is being recognised as emergency cases among the many other sick children waiting for care. Even if they do get recognised, the clinical staff may not have access to appropriate diagnostic tools, treatment and monitoring to be able to manage the child, especially in often over-crowded and under-staffed units. If the critical care gap is to be filled, it must also be adapted to the context.


Palliative care is an approach to alleviating pain and suffering, and improving the quality of life of patients and their families when faced with serious or life-limiting illness. Palliative care emphasises comprehensive care supporting holistic needs, based on empathy and person-centred care. It includes comfort care and management of symptoms such as pain, and involves close communication with the patient – even very young children – and the family on how to adjust care when the child’s condition changes. When children are the patient, there may be a greater emotional burden for family members and the clinical staff treating them, and the child needs to be considered in the context of their family.


Whatever its extent, healthcare can deteriorate rapidly in acute crises such as conflict or man-made or natural disaster, with severe consequences for children. To reduce this risk, the emergency response may need to include vaccination to prevent an outbreak of a communicable disease such as measles; therapeutic feeding to treat severe acute malnutrition; or newly established outpatient services in a displacement or refugee camp, for example. Children in an emergency are also at increased risk of violence; separation from their families; abandonment; physical, psychological and sexual abuse; economic exploitation; and neglect. The humanitarian response must include measures to reduce this risk and ensure the safety and general wellbeing of children needing additional protection.

World Children’s Day 2023: Five wishes from MSF
msf.org.ukChildren are disproportionately affected by humanitarian crises, both directly – for example through the impact of conflict and disasters – as well as indirectly – through heightened vulnerability to consequences such as malnutrition and disease outbreaks.
For World Children’s Day 2023, we want to share with you our ‘wishlist’ for children and some of the work MSF is doing towards these goals. While some of the wishes may seem basic, the sad truth is that large numbers of children are currently facing failures in these areas. We strive to transform these wishes into a tangible reality for children in some of the most challenging environments.

MSF Paediatric Days
paediatrics.msf.orgPaediatric Days is an event for paediatric field staff, policy makers and academics to exchange ideas, align efforts, inspire and share frontline research to advance urgent paediatric issues of direct concern for the humanitarian field. Paediatric Days focuses on paediatrics because in humanitarian settings, children are the most vulnerable group, with the highest risk of disease and mortality. Visit the Paediatric Days website to learn more.
Visit MSF Paediatric Days website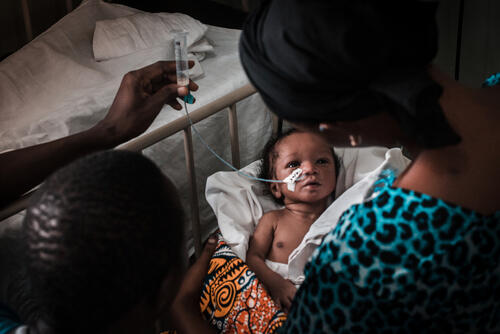
Paediatric emergency services in practice
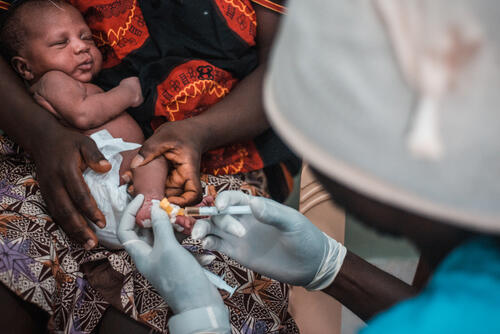
Five things to know about our emergency paediatric project in Bissau
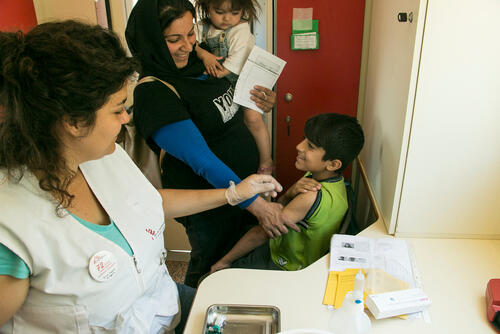
Vaccinating over 2,000 refugee children in Moria, Lesbos

Psychotherapy with children in Lesbos
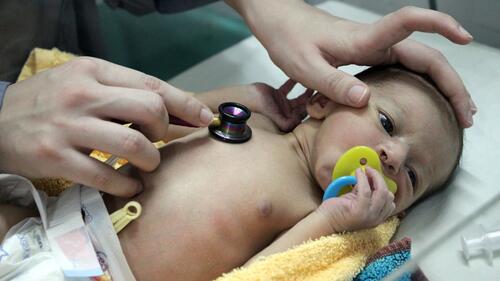
Increasing newborn babies' chances of survival

A name full of hope

“My sister, I will take care of you”

Illustrating MSF’s busiest maternity ward

Critical humanitarian situation unfolding among internally displaced people in Bama, Borno state

MSF Field Research
We produce important research based on our field experience. So far, we have published articles in over 100 peer-reviewed journals. These articles have often changed clinical practice and have been used for humanitarian advocacy. All of these articles can be found on our dedicated Field Research website.
Visit site



