Nineteen Central Africans, including three MSF staff members, were killed during an armed robbery in the grounds of MSF’s hospital in Boguila, Central African Republic, on 26 April 2014. One year on, an MSF team in Boguila continues to answer people’s medical needs in an area where insecurity and violence persist and no other healthcare is available.
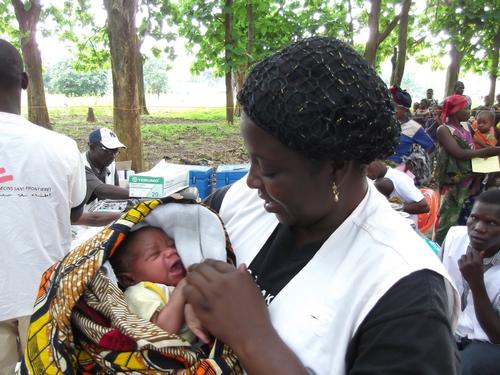
It’s an ordinary Friday morning at the MSF-supported health centre in Boguila, in the north of Central African Republic (CAR). Christelle, 19, arrived in the early hours of the morning and gave birth at 9.30 am with no complications. The baby – her second – is a healthy girl of three kg. By lunchtime, after the baby has had routine vaccinations, mother and child are able to join their family again, though they will come back to the centre for postnatal check-ups.
Christelle is one of almost 90 women who gave birth in the MSF-supported health centre in the first two months of this year. She lives nearby, in Boguila town, but many pregnant women come here from much further away, to give birth or to get help after a complicated home birth in which they may have haemorrhaged or developed an infection. They arrive by bike, motorbike or on foot, even at night and from as far as 50 km away.
“Women suffer a lot. When a new baby is born, it’s a moment of pain, but also of happiness,” says Rachel Ndoyan, midwife and mother of six. “I fight with MSF against mortality in Boguila. The most important thing is that we do it providing free healthcare.” In the same hospital where 19 people were killed one year ago, life prevails.

Immediately after the tragedy, MSF made the decision to reduce its activities . Now it functions as a health centre rather than a hospital, with a team of Central African staff providing outpatient consultations, including reproductive healthcare, vaccinations and treatment for malaria, malnutrition, HIV and tuberculosis (TB). People’s health needs remain as urgent as ever in an area where there is no other medical care available.
“Malaria is the main disease, especially for children: half of our patients testing positive are under five years,” says Elysée Tando, supervisor of the health centre. “Respiratory tract infections are also a common problem, together with parasites and, amongst the younger patients, diarrhoeal diseases. People spend a lot of time in the fields for the harvest, or in the bush for fear of the violence, with consequences for their health. Sometimes they are also afraid to travel here.”
Whenever there is the rumour of an attack by an armed group, the whole community is united in fear, with both patients and health centre staff fleeing into the bush to hide. Insecurity in Boguila as in many areas of the country restricts the movements of MSF’s teams and makes it hard for them to reach people in hiding. As a result, MSF looks for other solutions to provide medical aid to people living in remote areas. In the areas around Boguila, MSF is supporting four health posts where medical staff detect malaria patients at an early stage of the disease. They do the same at Boguila health centre, referring the most severe cases to the nearest hospital, which is run by MSF in Paoua, two hours drive away.
MSF has been working in Boguila since 2007. In 2014, the team carried out 194,157 medical consultations, more than 80 percent of them for malaria, and assisted 453 deliveries.
MSF has been working in Central African Republic since 1997, and currently has more than 300 international staff and more than 2,000 Central African staff in the country. In response to the crisis, MSF has doubled its medical projects since December 2013, and is running some 20 projects, including some for Central African refugees who have sought shelter in neighbouring countries including Chad, Cameroon and Democratic Republic of Congo.
Voices from Boguila
1. Lois, 37, assistant nurse, with MSF since 2009
“The day of the incident at the hospital was terrible – the worst day of my life. While I was still at home, getting ready for work, I saw some cars arriving in Boguila and later I heard gunshots. Now, when I hear loud noises nearby, I am afraid and I want to escape. I have already run away a couple of times over the past few months, when there have been rumours of armed people arriving in town. I’ve also had to flee with work colleagues to the bush for several hours. It´s very hard to work like this, but people’s health needs are huge, and MSF is the only health provider. Lots of patients come here, many of them children. Without healthcare, without MSF in Boguila, our children would be like dead leaves falling from a tree.”
Gladice, 35, midwife assistant, with MSF since 2006
“During the attack, I was having a break at the house near the hospital. The gunshots became louder and more intense. I was so afraid – I thought it was the end of my life. We stayed on the floor for 45 minutes. Only when it was silent were we able to go and see what had happened. On the way, a colleague told us of the death of another colleague and asked us to go and check on the wounded. We brought three of them, still alive, to the inpatient ward for treatment. I keep working with MSF in order to help my people, who desperately need healthcare.”
MSF144274 Gladice holding “Little Gladice“ is brought for a medical check up at one of MSF’s mobile clinics near Boguila.
3. Ghislain-Serge, 37, lab technician, with MSF since 2006
“One of the colleagues who was killed was my friend. I stayed for two days to organise the laboratory, and then I went back to Bangui. My family is there, including my brothers, sisters and cousins. The day I arrived in Bangui, a man was killed in the street near me as I made my way home, and my cousin pointed out that this was no different from what I had experienced in Boguila. Violence is everywhere. After the incident, I didn’t think about stopping working for MSF, but I did reflect on the risks and whether I wanted to continue taking these. I realised that in my country we are all at risk. I have known people die both from fighting and from illness due to a lack of medications and healthcare. I want to keep working with MSF. By doing so, I can continue to develop as a professional, and I can provide support to the people in my country, who without MSF would have no access to healthcare.”