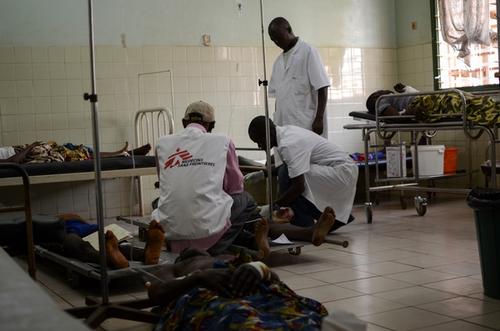
Jessie Gaffric is coordinator of Médecins Sans Frontières (MSF) project at the Bangui Community Hospital, Central African Republic (CAR), where the organisation performs emergency surgery for victims of the confrontations, abuses and violence rocking the city. Jessie has carried out several missions for MSF in violent and conflict settings, including Yemen and the Democratic Republic of the Congo. However, her mission in the CAR is the “most difficult” to date. Now returned, she describes the situation there.
Who are MSF’s patients at the Bangui Community Hospital? What kinds of wounds have they received?
In Bangui, we treat primarily men, between the ages of approximately 20 and 35. Most are combatants. Women and the elderly make up a minority of the patients. They happened to be in the wrong place at the wrong time. Children under the age of 15 were treated at another facility – the Bangui Pediatric Complex.
However, a large majority of the patients who came from outside the city - from villages in the provinces that that been burned and looted and who are transferred by the ICRC or other MSF teams to the community hospital – were women and children.
Nearly all of our patients are victims of violence. The most common injuries are bullet and grenade wounds, followed by then knife and machete wounds. The next category includes victims of lynching, confinement and torture, and, last, people who have been wounded while fleeing. The type of wound is always nearly the same, even if the number of grenade and knife wounds and cases of confinement and torture rise at specific times, based on the nature of the fighting.
What were the obstacles and constraints that you faced in your work?
Insecurity is the main problem and that’s what makes it hard for us to do our work. For example, we have to manage our time differently. Our teams cannot stay in the hospital after the 6 p.m. curfew. It's too dangerous. So we have to do a full day’s work during the 11 hours that we are there. Sometimes, we had to lock ourselves in the operating room – “hibernate” there – or evacuate immediately. Because of time pressures, we often had to postpone surgeries to the next day or, even, days later. The insecurity also meant that were few or no staff members at the hospital at night. When it was time for us to go, we had to leave patients alone, without medical monitoring. We didn’t know whether they’d be alive when we returned.
On days when there was fighting and we were likely to receive a large inflow of wounded patients, the city was more dangerous. Hospital employees couldn’t leave home to come to work. We then had to manage as best we could with the MSF expatriates and the few Central Africans who had slept at the hospital. The days that involved the most work were generally the days when we had the fewest people available.
As project coordinator, you were responsible for the teams’ security. How did you manage that?
It took a huge amount of time. The situation was chaotic - between the armed men who came into the hospital, armed patients, and family members and visitors – also possibly armed – who were always coming and going. Some categorically refused to turn over their weapons at the hospital entrance. In any event, it was impossible to search everyone. Everyone was terrorized and very suspicious, which complicated things even further.
I had to step between them to prevent the lynching of a patient. The attackers looked at me with hate in their eyes.
Jessie Gaffric, MSF project coordinator
With Becky, the nurse in charge of post-operative care, we were constantly telling people, ”The hospital is a place where people come for medical care – conflicts must remain outside.” We talked with the patients a lot, as well as with everyone living on the hospital grounds. MSF places all patients together and does not distinguish based on group or religion. We had to talk to the patients about that policy and explain it to the families. That took a lot of time, too. But I think that in spite of the daily threats to the patients and the presence of weapons in the hospital, it allowed us to avoid serious problems. The populations respect our work and accept our rules. However, on some days, when we left for the night, we weren’t sure whether we’d find all our patients there the next day. It was awful.
The issue of security outside – around the hospital – is equally important. I was in constant contact with Thomas, MSF’s head of mission. I kept him informed about what was happening (for example, shooting or movements of armed groups) and he did the same for me. He provided tremendous support. For example, he would come to the hospital in the event of a serious incident or a surge of patients to help us manage the crowd. We made decisions jointly on issues like freezing team movements or evacuating the team when it was too dangerous in the hospital. It would have been much harder to deal with that alone.
Were you ever afraid?
Yes. Some of the armed men in the hospital frightened me. I had to step between them to prevent the lynching of a patient. The attackers looked at me with hate in their eyes.
I was also afraid when we traveled by car when there was shooting, when we would encounter combatants who looked really intimidating and when we saw corpses on the roads. I was afraid at MSF living quarters, too, when there was shooting in the neighborhood. That happened almost every night, but some nights were worse than others. We even had stray bullets enter the house.
I was also afraid of making the wrong decision when we were evacuating a team. And of my responsibility for their safety.
How was this mission in the CAR different from other MSF missions you’ve been on? How was it harder?
The constant tension and the complexity of the conflict. On my other missions, things were clear. This group was fighting that group. In the CAR, the clashes have developed into inter-communal conflicts. Everyone is fighting everyone today. The rise in violence, the levels it’s reached, the hatred that creates this fury to kill and mutilate – all of that was really hard. The wounds and the injuries, particularly knife wounds, were horrible.
The heavy workload. We had several large inflows of patients where a majority involved serious cases. That’s unusual. In Bangui, the percentage of serious cases was greater than that of minor injuries. Even “normal” days were much worse than what I was used to.
I think Bangui was the most difficult mission I’ve ever been on. Luckily, the team was great. We had a tremendous sense of cohesiveness, both at work and at the house. The Central African team worked very hard, too. That and listening to Janis Joplin at night - that's what helped us.
Is there a specific patient who particularly affected you?
There were several.
Idriss suffered a cranial trauma. His face was torn to shreds. He had to be strapped to the stretcher because we had to leave and he was very agitated. We showed the people who were there with him how to administer pain medication while we were gone. He died during the night.
Another man arrived, upright, walking, with his throat slit and his trachea open to the air. He also had machete wounds on the back of his neck and one ear had been cut off. He had been tortured for four days. He died the next day.
Then there was Michael, who had been stabbed in the throat and thorax. The entire team mobilized. He was stabilized and the surgical team did an amazing job. He’s doing well and can move his arm – which had been lifeless – again. That was a small victory!
All the patients in the orthopedic tent, too, who were there for weeks at a time, face to face, calm and in a pretty relaxed mood, despite their conflicts and differences. They had moved beyond what made them enemies outside.”