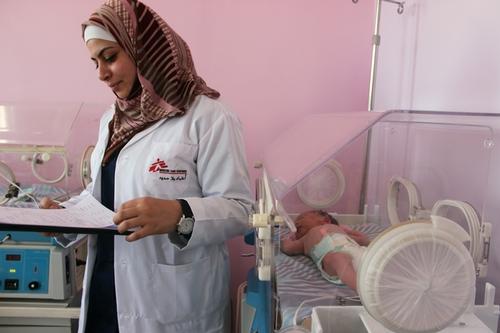
'Mass incoming casualties'
“Yes, I think many injured will be coming now.... perhaps we’d better call the surgeon.”
“Good idea,” I say after some time. It sounds stupid. I cannot think of a better reply. These were the words spoken by my assistant Ayyub* at 6.15 on a crisp July morning in northern Syria, as we peered toward the distant hills and listened to the sound of artillery echoing along the valley floor. These were the same words that I would hear often over the next two weeks, as more than 160 casualties – men, women, children – poured into our modest hospital. This was the first time Ayyub had uttered this prediction with such certainty.
Even after years of working in humanitarian emergencies, none of it has prepared me for standing on the roof of an old barn, perched on a hillside in what was ancient Mesopotamia, listening to the thud of nearby artillery, and trying to decipher what I am meant to be doing in response. Internally I can't even begin to fathom how glad I am to have this soothsayer standing next to me, someone who can practically inhale the morning air and understand what the day will bring. So yep: calling the surgeon – well, to be honest, calling absolutely everyone – does seem to be a good idea in this case. Pretty much the only idea in fact. But it's OK. This is what we are here for. I hope we're ready...
We down the sugary dregs of our tea and hurry below to the radio operator, Zafar, telling him to put the call out: “All hands on deck” – or in the parlance of MSF: “Mass casualty incoming.”
Abdomen injury
The first ambulance arrives before we’re ready. It's a pick-up truck with two wounded fighters – men from the frontlines – pallid, semi-conscious on mattresses in the back. A wave of young men – volunteers from the surrounding villages – surge into the truck and 20 hands float each patient onto a stretcher and inside to the emergency room, before re-forming at the hospital gates to wait for the next ambulance to arrive. The doctor on shift can see quickly one of the wounded men needs immediate abdominal surgery. It's complicated. It's messy. Massive injury to the abdomen: his chances are fair at best.
William, the surgeon, arrives at 6.30 am, barely minutes after the first wounded men. With 20 years experience with MSF, a 6’4” frame and a naturally calm disposition, he's a gangly rock in the middle of the hectic buzz. Accompanied by the anaesthetist and the operating theatre nurse, he's scrubbed up in less than five minutes and in the theatre operating on the man with the hole in his gut. An hour later, practically everyone we employ has arrived: about 90 local staff – doctors, nurses, midwives, drivers, guards , clerks – and 12 international staff – mostly medical professionals – all working flat out or pitching in in some way, whatever way they can. The hospital is swarming with people.
It's shameful, but I realise now as I write that I don't know the outcome of that first patient in surgery that morning, whether he survived or not. I lost track of him and countless others as injured men and women continued to arrive all day, the sound of artillery filtering over the beep-beep of medical equipment as beds, and then the floor space, filled up with the injured and the dying.

"The hardest day"
The surgical team worked until three am the next day. They worked straight through. Maybe sat down for 30 or 40 minutes in total. Eight operations, I think. And this continued for the best part of two weeks. “That was the hardest day of surgery I've ever had,” William told me after that first day, and he meant it. Thankfully, I never had to hear him say that again. Even though he conducted over 40 more surgeries in the following days, never were those days as hard as that first one.
But here's the catch. This isn't the most important work that MSF is doing in Syria.
This is not where the most lives are being saved, or the most suffering is being alleviated, or the most human dignity is being defended and upheld. But it makes for a more interesting narrative. Right?
Instead, I could write about 60-year-old Mohammed Asghar, who walks 2 km every fortnight through the valley to receive his diabetes medication and, whilst he's at it, to sit for a few hours with other old-timers in the tea shop to catch up on local gossip. Or I could write about expectant mother Selma, and her doting husband Basam, who spend a worrying month in the maternity ward with pre-eclampsia before Selma gives birth to a healthy baby girl. I could write about that, but I don't really have the skill to depict such human stories with interest or, more importantly, the fidelity or sensitivity they deserve.
People trying to lead ordinary lives
But I do want to try to explain that it's underneath all of this drama – the bombs and the bloodshed and the headlines – that there are people – just people – all trying to live their lives and continue from day to day. People who want to tend their land, or attend school. Look after aged parents, or grow up to become a dentist, electrician or writer. Give birth, find love, find happiness. Seek security for the family, or a new place to live now that there is a baby on the way. All the things that people do, all over the planet, every day. But doing this in a country at war. Trying to continue a life as conflict grinds on. And each day the reserves, emotional and material, are worn down layer by layer until they are spread so thin you don't know what to do anymore. Friends lost, brothers gone, families split or broken.
And this is where MSF and, to be honest, several other independent, neutral organisations are making a difference. A very small difference, but a difference nonetheless. MSF is providing healthcare for people where the previously functioning health service has, in some cases, all but evaporated. MSF provides maternity care for pregnant women, mental health services for the bereaved - imagine a war starting in your city, town or village - medication for the sufferers of chronic illnesses such as diabetes, or antibiotics for simple infections, that if left untreated can become life-threatening.
Those two weeks of mass casualties, in which, yes, many lives were literally saved on a surgical table, were in fact preceded by six months of relative calm in the emergency department. The calm was despite the fact that we were covering perhaps 90 percent of all health needs for a catchment population of approximately 100,000 people. Try asking the midwife on-call if she was bored in that time.
And providing this healthcare genuinely helps people maintain some control and dignity in their lives.
*All names have been changed to protect identities.
People who want to tend their land, or attend school. Look after aged parents, or grow up to become a dentist, electrician or writer. Give birth, find love, find happiness.Adam Sharp