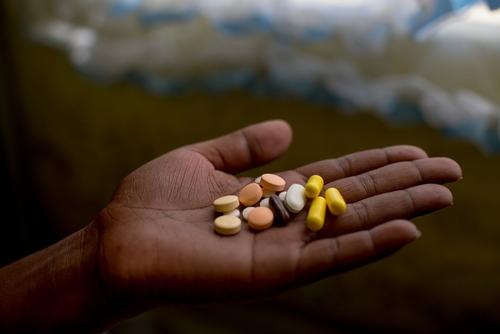
Current treatment regimen: bedaquiline, delamanid, linezolid, clofazimine, levofloxacin, ethambutol, terizidone
Nonyanyiso Baloi, a 32-year-old mother of three, lives with her children and aunt in Khayelitsha, Western Cape, in the same house she has lived in since 1989.
At the beginning of April 2016 she started showing symptoms of tuberculosis (TB). A chest x-ray at her local clinic suggested she had TB and doctors started her on regular treatment immediately.
"I lost weight, had no appetite and was vomiting a lot. I was always tired," Nonyanyiso says. The illness made it difficult for her to take care of her eight-, six- and four-year-old children, to whom she is a full-time mother.
At first, Nonyanyiso's liver reacted badly to the first-line TB drugs she was given and she developed severe jaundice. She was switched to a three-drug 'liver-friendly' regimen – which includes the injectable drug kanamycin – with a plan to reintroduce the regular drugs individually while her liver recovered, explains MSF TB doctor, Dr Jennifer Hughes.
"Unfortunately she developed hearing loss only four days later, so the kanamycin was stopped on 17 April 2016, leaving her with just a few treatment options," Dr Hughes says. "Then a delayed sputum result finally reached the clinic on 19 April: she actually had multidrug-resistant TB (MDR-TB)."
Nonyanyiso's liver function improved sufficiently by early May that her local doctor applied for newer TB drugs through the Department of Health, including bedaquiline, as an alternative to the injectable agent which had caused the hearing loss.

"While waiting for the drugs to be approved, she developed deep vein thrombosis in hospital and had to receive a blood transfusion due to severe anaemia," says Dr Hughes.
"By mid-May, just before starting the new medication, we received the final test results of the original sputum sample: she had pre extremely drug-resistant TB (pre-XDR-TB)! Nonyanyiso either had bad side effects from some drugs or the drugs were ineffective against her drug resistance pattern – we desperately needed more options."
Nonyanyiso's doctors applied to MSF for delamanid to be added to the bedaquiline-containing regimen. At the end of May approval came through, and in early June, she started taking delamanid and bedaquiline along with five other drugs.
"When delamanid was added to her regimen, her sputum cultures were still positive, showing that TB was still actively growing in her lungs. However, once established on an effective regimen, she has tolerated the treatment well," Dr Hughes explains.
"Today Nonyanyiso has overcome the worst and is on the road to recovery. In August, her sputum cultures were confirmed negative and we're waiting for the September results. She'll need to continue treatment and maintain negative sputum results for another 18 months before she can be declared cured."
Nonyanyiso is relieved: “I’m happy I got this treatment, because I couldn’t even walk back then,” she says, “but if I see myself now, I’m doing everything I couldn’t do before.”