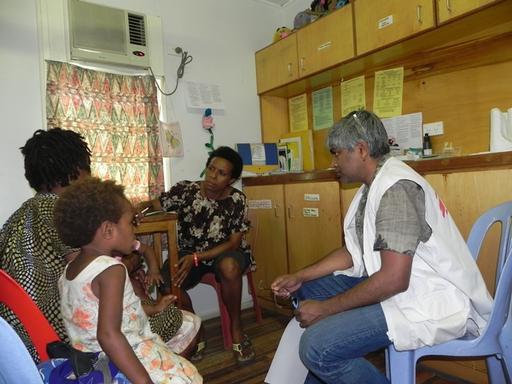
Every day, a woman in Papua New Guinea suffers the consequences of being raped and beaten by a member of their own family. This shocking reality and endemic problem is more devastating only because many women who experience this will not have access to essential medical and psychological support.
Visiting there, I was struck by the scale of the problem. My colleagues at Médecins Sans Frontières are running two family support centres in Lae and Tari, in the Morobe and Hela Provinces, and each day they are confronted with unspeakable trauma.
I met a number of women whose stories shocked me with the extent of the violence perpetrated, often at the hands of family members or within their own community. One woman’s story was especially disturbing. Walking home from the market with her daughter, eight men raped her on the side of the road. Her 6 year old daughter looked on. She told me at the time she was simply thankful that they hadn’t turned their attention on her child. Since the attack, she has experienced ongoing bouts of depression as she struggles with a family that has disowned her, blaming her and accusing her of encouraging the men who attacked her. She came to the Médecins Sans Frontières family support centre after subsequent beatings and abuse at the hands of her husband. This was her fifth time at the clinic. Her injuries were extensive.
Despite all that this woman has suffered, at least she has found what many other survivors in her situation in PNG have not: medical and psychological care. Through regular visits to the support centre she has been able to get the treatment that she needs. Many other women in her situation - maybe even the majority – do not have access to these services. My colleagues treat survivors every day with their own such experiences, but we know that, outside the two provinces where we work, many more are left without access to essential medical and psychological care.
However, we have no way of knowing the true extent of the problem, as national public health statistics continue to lump accidents and injuries in the same category as violent trauma and rape. That means someone who has been in a traffic accident will be classed in the same category as a woman who has been raped, or a child who has been beaten. The most commonly cited estimate based on decades-old government studies indicates that 70 percent of women in PNG experience violence, but these figures have not been updated in a nation-wide study since. Moreover, regular public health reporting from health centres and hospitals around the country does not separate data, so there is no way to track whether the situation is improving or worsening, in any given location.
Between the two projects in Lae and Tari, we treat around 60 sexual violence cases a month. This is an unusually high level of such violence for a country which is not experiencing any ongoing open war or conflict. Government and community efforts to tackle the problem have focused on obtaining a measure of legal and financial redress for victims of violence, but too little attention is paid to the medical emergency these incidents represent for each individual patient.
All women who survive family and sexual violence need access to five essential services in order to assure their own health and the health of their families. These are the same services we provide in our clinics in Lae and Tari: emergency medical care for cuts and other wounds; emergency psychological first aid; prevention of HIV infection, with post-exposure prophylaxis, and treatment for other sexually transmitted diseases; prevention of unwanted pregnancies with emergency contraception; and prevention of Hepatitis B and tetanus through vaccinations. Importantly too, our family support centres provide women with a space where they can be heard, safely and confidentially.
Patients need these services to be available in one location, for free, in order to ensure they really do receive the care they need as soon as possible after any incident. This care is time critical – if a woman does not get the medical treatment she needs within days of an incident, her chances of contracting HIV or other diseases increase substantially. And as we have seen in many countries, HIV prevalence can, and does, destroy the social and productive fabric of a country and its workforce.
We cannot ignore the societal and economic implications of family and sexual violence. Treating family and sexual violence as a medical emergency ensures not only that the survivor is cared for immediately, but also may help reduce the long-term impact of this violence on families and communities throughout PNG.
While in PNG I met with the Deputy Prime Minister and the Secretary of Health, among other key officials. They are aware of the problem. We asked that the government do more to ensure all of these five essential services are available in at least one location in each province – and to ensure that public-health data on violence are disaggregated. This will help the government itself, and any partners interested in addressing this crisis with them, to see where progress is being made and where more attention needs to be focused. This is one clear ask of government that can be acted upon without delay. We are ready to assist in this task. The last thing anyone wants is for survivors of family and sexual violence around PNG to suffer in silence without the essential services they and their communities so urgently need.