While significant progress has been made in South Africa since the first Durban conference in 2000, deadly and unnecessary HIV treatment gaps persist in other countries
Durban, South Africa – Médecins Sans Frontières (MSF) is calling on global HIV/AIDS leaders at the International AIDS Conference in Durban to develop and implement an action plan to address the critical lack of access to HIV treatment in those countries in West and Central Africa where coverage remains below 30 per cent. This comes as new MSF data from Southern Africa suggests that the implementation of “Test and Start” is feasible but that community-led outreach is necessary to test and link people living with HIV to care and support them on lifelong treatment.
This situation in several countries in West and Central Africa is reminiscent of MSF’s call at Durban 2000 to expand access to affordable antiretroviral drugs in South Africa, where more people than ever are now living long and healthy lives on treatment. As we’ve seen, civil and community support and affordable medications play a key role in making sure people get and stay on antiretroviral therapies. Failing to reach people in neglected regions puts at risk global goals to reach 30 million people with treatment by 2020 and achieve UNAIDS 90-90-90 targets.*
In MSF’s project in Swaziland, data from across nine health facilities in rural Nhlangano district showed that of people who started treatment with a CD4 cell count above 500, 90 per cent were still on treatment after six months. In MSF’s project in KwaZulu-Natal (KZN) province, South Africa, when offering treatment including to people with higher CD4 counts, over 80 per cent of people remained on treatment after twelve months, whether they had started treatment below or above CD4 350. Initiation rates remained stable for people at CD4 levels below 350. These findings suggest that newly-eligible patients will initiate and remain on ART if provided the opportunity, without compromising access to care for the sickest people.
However, testing and offering people treatment and ensuring life-long adherence will not be possible without outreach activities that target testing people before they are ill. Community testing strategies piloted by MSF in KZN are particularly effective at reaching first-time testers, including students, young women at risk of HIV, and young men who may not attend health facilities. Door-to-door testing by community health workers reaches people of all ages, and can even be less expensive than facility-based testing. Importantly, people diagnosed at mobile and stand-alone sites in 2015 had higher median CD4 counts (462 cells/mm³), compared to those diagnosed in facilities (CD4 363 cells/mm³).
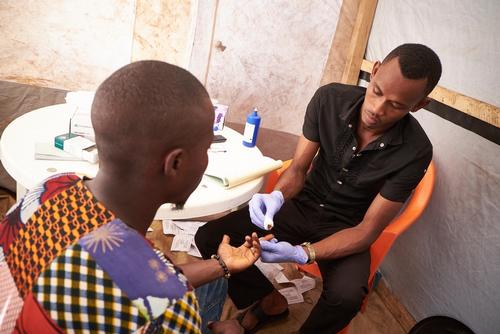
“Patient care works like dominoes, with an entire community involved in testing people where they live and work, and ensuring someone who tests positive is initiated on treatment, and supported to stay adherent to lifelong treatment with suppressed levels of the virus,” said Musa Ndlovu, Deputy Field Coordinator for MSF in KwaZulu-Natal. “The lay workers in communities and facilities are the glue holding everything together - improving both quality of care and access. We need governments to ensure that a workforce of lay people is employed, maintained and expanded throughout the region, to provide testing, treatment initiation and adherence support for all who need it.”
While policies and practices for employing lay workers vary widely, when they are absent from the health system, the impact is substantial. After lay counsellors were withdrawn from facilities in KZN province in two waves during 2015, the monthly average number of HIV tests conducted in facilities MSF supports in Eshowe/Mbongolwane decreased by 25 per cent and a further 13 per cent respectively. The number of new people starting on treatment in the area also declined by 20 per cent in 2015.
Adopting community-based strategies could help expand coverage in West and Central Africa where barely one in four people among the 6.5 million with HIV in the region have access to treatment. Nearly one third of AIDS-related deaths globally occur in the region, and in order to achieve the global goal of reaching 30 million people with treatment by 2020 – agreed by all governments at the UN in June – an additional 13 million people need to be reached with treatment, one third of whom live in West and Central Africa.
We need a massive booster shot for West and Central African if we’re going to get anywhere close to achieving the global treatment goals.Dr. Eric Goemaere, HIV/TB Unit Coordinator for MSF's Southern Africa Medical Unit
At a hospital where MSF works in Kinshasa, Democratic Republic of the Congo, one quarter of people with HIV arrive too sick to be saved, with 39 per cent of these dying within 24 hours of being admitted to the hospital. In Central African Republic, although national HIV prevalence is believed to be below 5 per cent, 84 per cent of deaths in Beberati hospital where MSF works are related to HIV/AIDS, while in the north of the country in Ndele, Kabo and Batangafo, MSF teams report HIV positivity rates of 33 per cent at the VCT level.
“The HIV situation in West and Central Africa reminds us of the terrible days over a decade ago in Southern Africa, when people were dying and no treatment was available,” said Dr. Eric Goemaere, HIV/TB Unit Coordinator for MSF's Southern Africa Medical Unit. “Solutions to close this massive treatment gap exist. We need a massive booster shot for West and Central African if we’re going to get anywhere close to achieving the global treatment goals. When there are so many millions of people on treatment today, the right to access that lifesaving treatment should not depend on where people live. We cannot leave these people behind.”
*UNAIDS 90-90-90 targets aim that by 2020, 90 per cent of people living with HIV know their HIV status; 90 per cent of those people are on antiretroviral treatment; and that 90 per cent of those on treatment have achieved ‘undetectable’ levels of virus in their blood (viral suppression).
MSF has been providing antiretroviral treatment to people living with HIV/AIDS since 2000, and currently supports HIV treatment for nearly 247,000 people in 19 countries.







